Northants Guide Dog And Robot Best Friends After Date
A guide dog has conquered her fear of delivery robots after going on a date with one.
Amelia, a Labrador from Raunds in Northamptonshire, reacted badly to Levi the robot when they crossed paths during a walk.
The delivery company that owned Levi invited Amelia to its depot to try to break the ice.
And Amelia’s owner said the technophobic dog was now taking electronic couriers in her stride.
White boxes on wheels with aerials sticking out of them have become a common sight in some towns and cities as they trundle down pavements and across roads delivering takeaways and packages.
But David Holmes, Amelia’s owner, discovered that, while the robots may be familiar to most people, they were new to Amelia.
He said: “Amelia took me to the kerb, and she started barking, growling and pulling me into the road.
“I heard a little trundling noise behind me. Obviously, I didn’t know what it was, and when I got home, my wife said to me ‘did you meet the robot?’ and then it all clicked.”
Mr Holmes posted about his experience on social media and it came to the attention of Gareth Chisholm, general manager at DPD’s depot in Milton Keynes.
He said; “I wanted to reach out to see if we could do any sort of acclimatisation and make the dog and the robot best friends.”
He brought them together at the depot to see what would happen.
He said: “We didn’t really have a plan of how we were going to introduce them – we knew we had to do it slowly with treats.
“She started off very apprehensive, but once the treats came through, she got more involved to the point where we were able to walk the robot past Amelia with very little reaction and she got more and more accepting of it being in the area.”
The tests were then repeated on a pavement outside the depot, to reflect a real-life environment.
Amelia passed with flying colours. She did not react to Levi’s presence.
Soon afterwards, Mr Holmes discovered that the familiarisation session had really worked.
He said: “I went out for lunch and I had my wife with me and she said there was a robot there.
“Because Amelia didn’t react, I didn’t know.”
Last item of the day
some of the early evening for you https://amzn.to/3wk0bzg
item of the early evening for
Amazon private Pinterest update for you
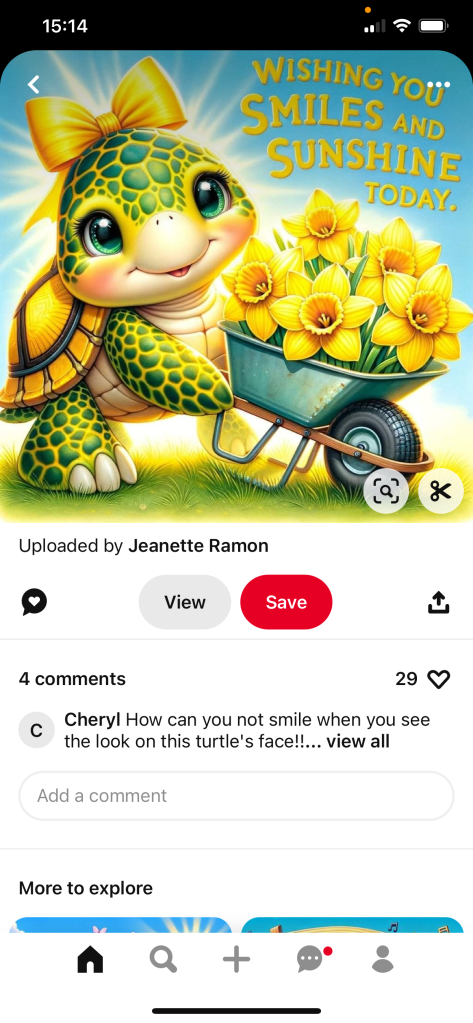
second positivity painting/saying good day for you all
positivity saying of the day for you all
Guide Dogs Taught To Deal With Delivery Robots
A sight-loss charity is teaching trainee guide dogs how to deal with delivery robots after owners reported their pups were unnerved.
The Guide Dogs training centre in Leamington Spa has teamed up with the firm behind the tech so dogs-in-training could be familiarised with it.
Starship Technologies donated a robot shell to the charity and pledged to support working dogs reacting to the machines on the streets.
Staff at the charity said they were “really pleased” with the progress already made by apprentice guide dog Vinny, external.
Autonomous six-wheeled delivery bots travel on pavements to deliver food, groceries and packages.
They were introduced in Milton Keynes six years ago and since expanded to towns around the UK, with firms such as the Co-op and DPD opting in.
Guide dog trainer Paul Lennon explained a couple of service users had highlighted dogs’ “strange reactions” to them.
“We expect the use of them to really go up over the next few years,” he said.
“We really wanted to have a training aid [to make sure] they’re not going to be held back by things that they meet on the streets.”
Golden retriever Vinny’s training introduced him to the static bot in a room strewn with boxes, toys and sniff matts, with movement incorporated later.
Scattered treats fostered a “positive association”, Mr Lennon explained, adding he was “really pleased” with the two-year-old’s progress.
“We’ll do this time and time again just to make sure that the dogs are really happy with it,” he said.
Ryan Holroyd-Case from Starship Technologies said its partnership with the charity would deepen their understanding of how guide dogs interacted with the tech.
“Over the years we’ve conducted testing with guide dogs to observe their reactions,” he said.
“We’ve found many dogs work very well around our robots without distraction, but some need a little more support.”
The Leamington-based guide dog training centre is the largest in the country, supporting about 250 owners in the area.
“I was frustrated, lonely and unhappy during lockdown.”
That was the experience of Peter Livingstone during the pandemic, and he hopes the UK Covid-19 Inquiry will examine how people with learning disabilities coped.
He was speaking during an event to mark the inquiry arriving in Northern Ireland next week.
Peter, who is 35 and has disabilities, moved back to live with his parents during the pandemic.
He said being isolated from his friends during lockdown was tough.
“I was so lonely and when I had to go into hospital for treatment it depended on which matron was on if people were allowed in to visit me,” Peter said.
Not being able to see family members was stressful and sad, he added.
Peter hopes people with learning disabilities will be given a voice so lessons can be learned and views recorded for the future.
Senior politicians, health officials and key decision makers who were charged with guiding Northern Ireland through the pandemic will appear before the UK Covid Inquiry from 30 April to give evidence.
Secretary to the inquiry Ben Connah said he wanted local people to continue coming forward to tell their stories and help shape the final report’s recommendations.
Speaking at the Ulster Museum, where an exhibition marks key moments of the pandemic, Mr Connah said the inquiry’s presence in NI was important.
“The inquiry will be examining the core decision making in NI and hearing stories from members of the public to help the inquiry build a fuller picture of how the pandemic affected local people and the UK as a whole,” Mr Connah said.
He said it was not too late for people to get in touch.
Bereaved Families for Justice in Northern Ireland have said they are not satisfied with aspects of the inquiry and have called for Northern Ireland to have its own separate investigation.
Mr Connah, who has met families on numerous occasions, said he had tried to reassure them that their stories and concerns were important and key to the inquiry’s overall findings.
The UK Covid Inquiry was established in June 2022 to examine the UK’s response to and the impact of the Covid-19 pandemic and to learn lessons for the future.
It was established as a direct result of campaigning from Covid Bereaved Families for Justice who had been calling for a wide-reaching statutory inquiry that would establish the truth about how so many people lost their lives and whether any deaths could have been prevented.
Module 2c of the Inquiry will look at how the structures within NI responded and communicated with the UK government, decision-making, public health response, decisions made and by whom and how those decisions were informed.
adopted not saying for you puppy lovers
cute dog pay for your nighttime
sing for the nighttime
good night Sally
of the evening
item of the evening
children girls early item of the day
CP Man Runs Six Major Marathonx
A difficult birth left Andrew Tomlinson with a brain injury which made his chances of ever walking slim.
But more than 30 years later, he believes he is the first runner with cerebral palsy to complete all six of the world’s major marathons.
On Sunday, the 40-year-old from Glasgow crossed the London Marathon finish line in under four hours.
He has previously completed races in New York, Chicago, Tokyo, Boston and Berlin.
Andrew said building up to the London race had taken three years of his life.
“At the end I was fighting against all the emotions – pride, joy, finishing … but also sadness too, because it’s finished.
“I wanted to go back to the start.”
Andrew has hypertonic cerebral palsy, which means he suffers from tightening muscles and regular spasms.
It affects his the mobility down the left hand side of his body and means he walks with a visible limp and has slurred speech.
He receives regular treatment as symptoms can flare up, causing him severe discomfort.
“It’s one of the worst pains,” he says.
He says keeping active also helps control some of the pain, making it more bearable to live with the condition.
“Running also hurts but I’ve noticed that the more I run the less the cerebral palsy hurts, so it’s actually helping me,” he says.
There are about 16,000 people with cerebral palsy in the UK, and it affects everyone differently.
Along with the physical impact of the condition, Andrew has also suffered socially, which is why he made the decision to take up running.
He says cerebral palsy can often isolate him from others. In 2019 he realised that he’d got himself into a rut and that something had to change.
“I’d come home from work and play a games console by myself and one day I thought I really have to challenge this, cerebral palsy was winning.
“I spoke to a friend who suggested I try a marathon. I thought, I don’t even know if I’ll manage a 10k, let alone a marathon.”
Marathon ‘miracle’
Within six months, Andrew had travelled to Berlin to complete his first world major marathon. The next year he joined his local road running club, which he says enhanced his life.
“I now have a hobby and a social life,” he adds.
His mum Linda says that the fact Andrew is able to walk, let alone run marathons, is a miracle after a difficult birth left him with damage to his brain.
“He had lack of oxygen to the brain but we didn’t realise at first,” she says.
“When he was one we noticed he wasn’t using the left hand side of his body. I took him to the doctor who referred him to a specialist.
“It was then we were told he has cerebral palsy and that he might never walk.”
‘A true inspiration’
Linda took medical advice and Andrew attended physiotherapy at Glasgow’s Yorkhill hospital for sick children.
Within two years he took his first steps.
“He tripped up and fell often, even today he struggles – but when he does fall he gets straight back up again.
“But running seems to have the opposite effect. When he runs he relaxes, it’s like he’s not got cerebral palsy.”
Linda says she worries about Andrew on his solo travels around the world completing marathons, but knows he’s doing what he loves.
“He puts an awful lot of work in, he never complains and he tries so hard to keep himself mobile.
“He’s a true inspiration.”
Women With Learning Disabilities Star In Menopause Film
A film has been made by and for women with learning disabilities or autism to explain that perimenopause and menopause symptoms are not “embarrassing or scary”.
Ace Anglia, based in Stowmarket, has worked with Suffolk Libraries to share what happens before and after periods stop. The film features women supported by the organisation.
Nicole Smith, from the libraries’ Menopause and Me Project, external, said the aim was to “reflect different experiences” and to show people they were not alone.
Women in the video, external explain that moods can change, you can forget things, and symptoms are different for everyone.
Shenah, who features in the film, said: “People with menopause matter. Making more people aware of menopause is really important.”
Rae, who was also filmed, said: “It is important to make this film for women who are about to go through menopause to understand what it is and how it changes your body.”
The video explains that it is “natural”, that having a healthy diet or taking HRT can help, and that it can be beneficial to talk to support workers, friends or family members.
“The menopause is not embarrassing. It’s not scary. It’s natural. You can speak up about it. You are not alone,” the film explains.
Ms Smith said: “We want to reflect different experiences of the menopause and perimenopause in the resources we produce – whether that is from a sexual orientation, cultural or, in this case, learning disability and autism perspective.
“We want people to be able to not only identify with what they hear or read but also feel supported and, most importantly, not alone.”
A spokesperson for Ace Anglia, said: “We approached Suffolk Libraries to suggest creating some accessible information for women with a learning disability as part of the Menopause and Me project.”
Teams are also working to develop resources in more accessible and easy-to-read formats.
good night saying for everybody that likes saying of the day
Affiliate Amazon Pinterest update
positivity thing of the day for you all
public speaker talking about her disability story as a young teenage woman, positive disability stories and public speech of the day
glittery beautiful favourite painting of the day of a 😊
Disability Flying Lessons Launch At Kent Airport
A new programme of flying lessons for people with disabilities is “life-changing”, say student pilots.
Lydd Airport’s training centre and charity Aerobility launched the lessons in Kent on Thursday.
Instructor Al Rosser said lessons “give people a chance to do something they never thought they can do”.
Student pilot Ann-Marie Baldwin told BBC Radio Kent: “I’ve found my place in the world after taking up flying.”
The programme is open to people with both physical and learning disabilities, visible or non-visible.
Mr Rosser said when people fly they “forget all their other worries”.
He added: “They are the same as everybody else and it inspires them to go and do extra things in their life.”
Pilots receive specialist training to fly as Aerobility instructors in modified PA28 Warrior planes.
Stuart Miller, Aerobility facilities manager, trains instructors and club members how to use a hoist to help people into the planes.
He said he “caught the bug” after an experience session and has been flying solo since he got his private pilot’s licence in 2019.
He said: “For me it’s awesome, you can leave your disability on the ground, you are just another pilot in the sky.”
Ms Baldwin previously had to travel to Hampshire for her training and said being closer to home will make a real difference.
She said lessons are “amazing”, she “loves flying a lot” and she plans to volunteer at the airport.
She said: “Hopefully I can pick up stuff by being around other people, helping out and sharing my enthusiasm with other disabled fliers.”
Adrian Stephens, operations and safety manager at Lydd Aero Club said: “It’s great to see people smiling when they come down from flying whatever ability they are, having shared the joy of flying.”
Amazon affiliate links
Warwick Davis’ Wife And Hollyoaks’ Annabelle Davis’ Mother Samantha Davis Dies Aged 53
Samantha Davis, founder of dwarfism charity Little People UK and wife of Harry Potter star Warwick Davis, has died at the age of 53.
In a statement, the actor paid tribute to his “favourite human”, who died on 24 March, saying: “I miss her hugs.”
“Her passing has left a huge hole in our lives as a family,” he added.
Mrs Davis was also an actor, appearing alongside her husband in the final Harry Potter film in 2010, in which she played a goblin.
The couple met on the set of the film Willow in 1988, before marrying three years later.
The Star Wars star described Sammy, as he called her, as his “most trusted confidante and an ardent supporter of everything I did in my career”.
“She was a unique character, always seeing the sunny side of life she had a wicked sense of humour and always laughed at my bad jokes,” he said.
Davis said that with his wife by his side, he felt sure he could achieve anything, adding: “It was like having a super-power.”
“Without Sammy, there would have been no Tenable quiz show, no Willow series. No Idiot Abroad Series 3.”
He added it had been his wife who persuaded comedian Ricky Gervais to send him with Karl Pilkington for the travel series.
The couple’s children, Harrison and Annabelle, joined their father in paying tribute, saying “her love and happiness carried us through our whole lives”.
“Mum is our best friend and we’re honoured to have received a love like hers,” they added.
Davis played both Professor Flitwick and the goblin Griphook in all eight films in the Harry Potter franchise. He also played several characters in the Star Wars film series, and starred in both the Willow film and the 2022 sequel.
His wife’s other acting credits include the children’s series Through the Dragon’s Eye (1989).
Outside of acting, Samantha Davis and her husband founded the charity Little People UK in 2012 to help individuals with dwarfism and their families.
“She was passionate about helping people, without judgement. She had time for everyone and a genuine listening ear,” the Tenable host said.
Davis said in recent years his wife’s mobility had become impaired but she was “determined that it would not impact her quality of life”.
Disney, the network the Willow series was on, said Samantha was “beloved member of the UK film and TV community”, adding: “Our thoughts are with the Davis family during this difficult time”.
Hollyoaks actress Annabelle Davis shares her own tribute to her mother here.
Repair Shop Contestant Writes Fiction Book For LD Adults
A writer from south London has written a book inspired by the carousel horse in her garden, which was restored on the BBC show, The Repair Shop.
Author, Jennifer Munro from Sutton said Edward Pureheart and the Forever Children was the first novel aimed for adults with learning disabilities.
She wrote it for her 41-year-old daughter Kate Horncastle when she couldn’t find stories and entertainment suitable for her.
Jennifer hopes her book will raise money for epilepsy research so people like Kate will no longer have to take medications to manage the condition that causes seizures.
Kate has a rare genetic difference that causes epilepsy, autism and neurodevelopmental delays.
“We knew she had epilepsy, she had a very low IQ and she had autism, but we didn’t know why,” said Jennifer.
Following testing, doctors found that Kate had an extremely rare genetic difference.
“It’s called CHD2 deletion and they told me that there are only 270 other people with that diagnosis in the world.”
She hopes the book would raise funds to explore gene editing in epilepsy research.
“If they can figure out exactly what the gene deletion means, they can edit the genes and it’s possible that people like Kate won’t need epilepsy medicines anymore,” said Jennifer.
Edward – as he’s called – is the centrepiece of a sensory garden Jennifer created for her daughter to help keep her calm and happy.
“It was quite strange actually because she said this somebody is coming to your garden and she told me it was a horse,” said Kate.
“I said ‘you can’t have real horse in here’.
“A big truck came and he was in a box, brought on a ship – so it wasn’t a real horse – she was just tricking me.”
But after being out in the elements, Edward, believed to be at least 100 years old, had peeling paint and the wood was beginning to rot.
He was given a complete makeover and made weatherproof by restoration experts from the show.
Kate talks to Edward every day, communicating her needs through him.
The bond inspired her mother, Jennifer to write about his fictional adventures from a Texan fairground to garden in London, where he can only talk to children, or people who are neurodivergent.
She wanted to create entertaining stories suitable for Kate’s intellectual capabilities, but including themes she negotiates as an adult.
“I just thought ‘where is the magic for them?’
“Adult books are not appropriate, children’s books aren’t – you need something in the middle – something for them because they are unique.”
She added that there was no “mental age” for forever children – those who may never leave the nest once they reach adulthood.
“You can’t say ‘well she’s four’ or ‘she’s six’. She’s not – she’s many different ages all at the same time and in many different ways,” said Jennifer.
“Very seldom are they made to feel that their differences a good thing.
“But they are themselves – perfect and complete.
“Those themes are in the book too – about accepting each other the way we are and being loved for who you are.”
💔😂💞🫶🏼
disability story of the day raising awareness of spinal
out, enjoying the Sun three years ago on a walk😘🤣
Hotels ‘Should Offer Family Rooms For Wheelchair Users’
A woman has called for hotels to be more accommodating for families with a wheelchair user.
When Lizzy Simms, 44, and her partner Buzby Allen travel with their two children, they have often struggled to find an accessible room for a family of four.
Mr Allen, 64, has limited mobility and has used a wheelchair since experiencing a bleed on the brain last year.
Ms Simms, from Hopton, Norfolk, said hotel chains acted as though when someone got a wheelchair, “your children magically disappear”.
The family want hotels to provide rooms to enable children with a disabled parent “the chance to get away, like everyone else”.
Ms Simms has started a petition, external calling for hotels to be obliged to offer accessible rooms for families.
“What we are asking for really isn’t that much. It’s a wetroom and wider doorways,” she told BBC Radio Norfolk.
Kimberley Myhill, from Equal Lives, a disability rights organisation, said: “There is an assumption that disabled people don’t have money to spend.”
She said wheelchair users often did not stay at hotels due to accessibility issues.
Mickey Mouse, red jumper
item of the day for you all
Boy Surprised By Black Panther Teddy Bear With Hearing Aids
A boy who lost his hearing in both ears during cancer treatment has been surprised with a specially-made teddy.
Thomas was given the toy, based on his favourite Marvel character Black Panther, which has hand-sewn hearing aids attached – like the ones he wears.
It was created by audiologist Ruth Avierinos who wants to “reduce the stigma around hearing conditions”.
Thomas attends preschool at the Elizabeth Foundation at Queen Alexandra Hospital in Portsmouth.
His mother, Vicky, said: “It’s something to show him that although he might look different to other children, it’s normal and it’s OK.
“I don’t like to call it a disability. We call it his ‘magic ears’ and now he’s got his favourite character that also has magic ears.
“He has been taking him to bed every single night and, in the morning, he takes him back downstairs. Wherever he is, the Black Panther teddy is close by.”
Thomas is now in remission and spent Easter at home.
The Havant, Farlington and Waterlooville branches of Specsavers have been fundraising for the Sophie’s Legacy charity, based at the hospital.
The cause, which was set up after 10-year-old Sophie passed away from cancer in 2021, hopes to change the way children’s hospitals are run, with more play, nicer food for kids and parents, and to raise awareness of childhood cancer.
Ms Avierinos, who works for Specsavers in Havant, had been helping to raise money for the charity when she learned about Thomas, who has been wearing hearing aids since 2022.
She also donated 12 of her teddies to children who had to spend the Easter weekend at the hospital.
She said it was “such a pleasure to do” and her goal was “to reduce the stigma around hearing conditions and wearing hearing aids”.
How disabled people can live positive and productive lives and being positive about the fact that they are disabled
The UK’s first fully-blind overseas ambassador tells BBC News her disability can help build relationships with influential people around the globe, ahead of taking up a role in Slovenia in August.
Victoria Harrison has until the summer to become fluent in Slovene before taking up her post in the capital city, Ljubljana.
Learning languages is any foreign diplomat’s remit – but “disability prep”, as she calls it, is unique to her situation.
Getting used to a new home and memorising new routes to work and local cafes with her guide dog, Otto, are just some of the tasks Victoria has on her list alongside her day job.
“In my first [foreign] posting, I didn’t realise there was an amazing cafe very close to where I lived – because I’d walk past it and didn’t know,” she says.
Born with normal vision, Victoria developed an eyesight condition that gradually worsened throughout her teens.
She eventually lost her sight after university.
“It wasn’t always easy growing up with less good eyesight than other people,” she says – but she never felt her condition would hold her back from her dream job, diplomacy.
As a teenager, TV reports on the fall of the Berlin Wall, in 1989, sparked Victoria’s interest in the world of foreign diplomacy.
She asked her father what a diplomat did and learned they “get paid to travel the world, learn languages and represent their countries”.
“I thought that sounds fantastic,” Victoria says.
‘Really competitive’
In 1995, the Disability Discrimination Act, since replaced by the Equalities Act, was introduced to remove barriers faced by disabled people in employment.
A year later, Victoria’s first chance to work at the Foreign Office came in the form of an undergraduate work-experience scheme. Her main concern about her ability to do the job was not based on her disability, but her own insecurities.
“I thought maybe I’m not clever enough. I didn’t go to Oxbridge. It’s really competitive,” she says.
The Foreign and Commonwealth Office offered Victoria the internship in Moscow – but when she revealed she was registered blind, “there was a kind of silence… at the other end of the phone”.
“They then said, ‘we don’t have any blind people in our organisation’,” she says.
Victoria remembers feeling “surprised” rather than “disheartened” by the phone call.
She had always thought being a junior, or a woman, were more likely to hold her back in her career than being blind.
The placement was confirmed a few days later.
‘A novelty’
In 1997, Victoria got a permanent role in the Foreign Office – becoming the first person with a declared disability to work there.
“I was a novelty,” Victoria says.
“There weren’t [other] people who had significant disabilities.”
The Foreign Office was still finding its feet with the changes that came with the Disability Discrimination Act, and it took six months before Victoria was given a computer she could use.
“It wasn’t that people didn’t want to support me,” she says.
“It was just the fact that this was an organisation where we were… very much building the plane as we were flying it.”
Feelings of self-doubt crept in as Victoria noticed colleagues around her flourishing.
“I felt kind of frustrated because I thought I’m not able to show people that I’m actually as good as other people,” she says.
“And I didn’t really have a chance to prove the naysayers wrong.”
Some people even suggested to Victoria she had been given the role only because of “tokenism” or to bolster equal-opportunity statistics.
Attitudes in the UK slowly started shifting – but two years later, when Victoria was trying to land her first posting abroad, some foreign embassies had surprising reactions to her disability.
She remembers one saying: “This person needs to speak the language of the country – and obviously, being blind, they won’t be able to learn it.”
Victoria has since been on foreign postings to Helsinki and Sarajevo and says each new country presents unique challenges.
But she finds people often have a natural curiosity about her – and being blind can help with making personal connections while navigating the delicate art of negotiation.
“I might need to take someone’s arm to guide me to the way out of the meeting room,” Victoria says.
“That sort of thing brings a human connection that actually can be really helpful in building relationships.”
That connection can also help Victoria at work in other ways.
She is often self-conscious at work events that involve dining – and can become preoccupied with worries about things such as knocking over a wine glass.
At one such dinner, someone in the UK foreign secretary’s team noticed Victoria had picked up her knife and fork when the starter was served.
And they whispered to her it was soup, so she could grab her spoon instead.
“I just thought, ‘Thank goodness for that,'” Victoria says.
“But it also allowed me to focus on the fact that I actually need to be following the conversation, in order to write a report.”
‘Just cringe’
Victoria was the first blind person to join the Foreign Office, the first blind diplomat to be posted overseas and, after landing the Slovenia role, is now the first to become a British ambassador.
But asked what it feels like to be a trail-blazer, she laughs.
“It makes me just cringe thinking about it,” Victoria says. “Technically, yes, I’ve done a lot of firsts.”
But she adds: “I don’t like the word trail-blazer, because it sort of sounds like I’ve actually set out to be all of these things – and it’s kind of just happened.”