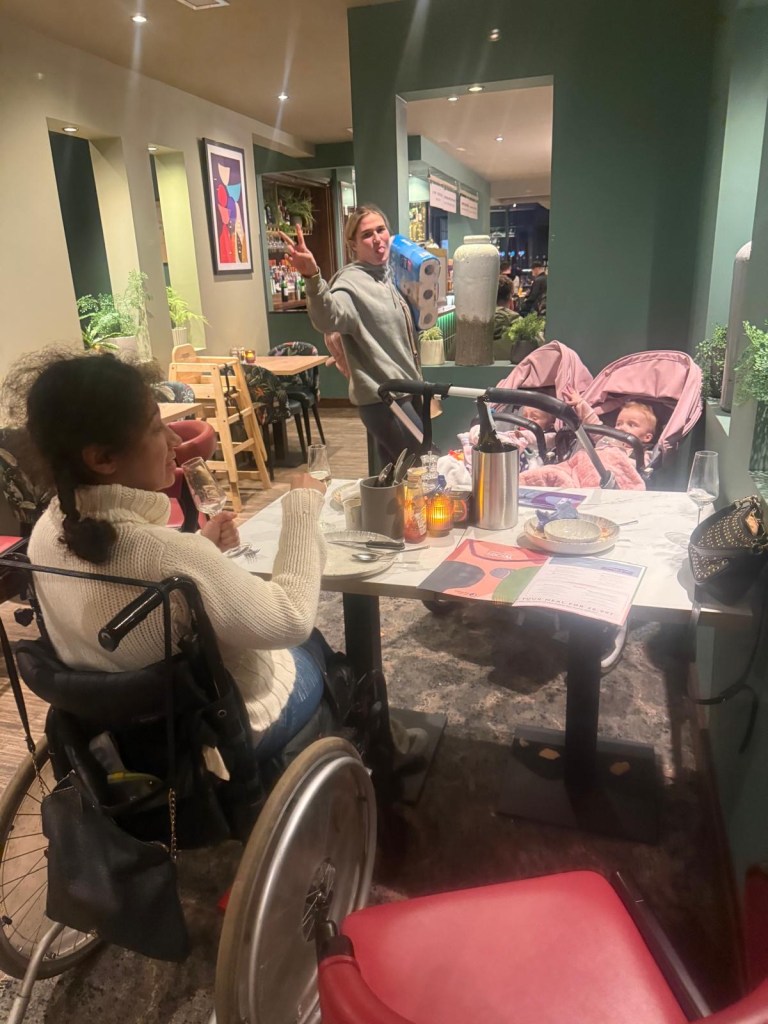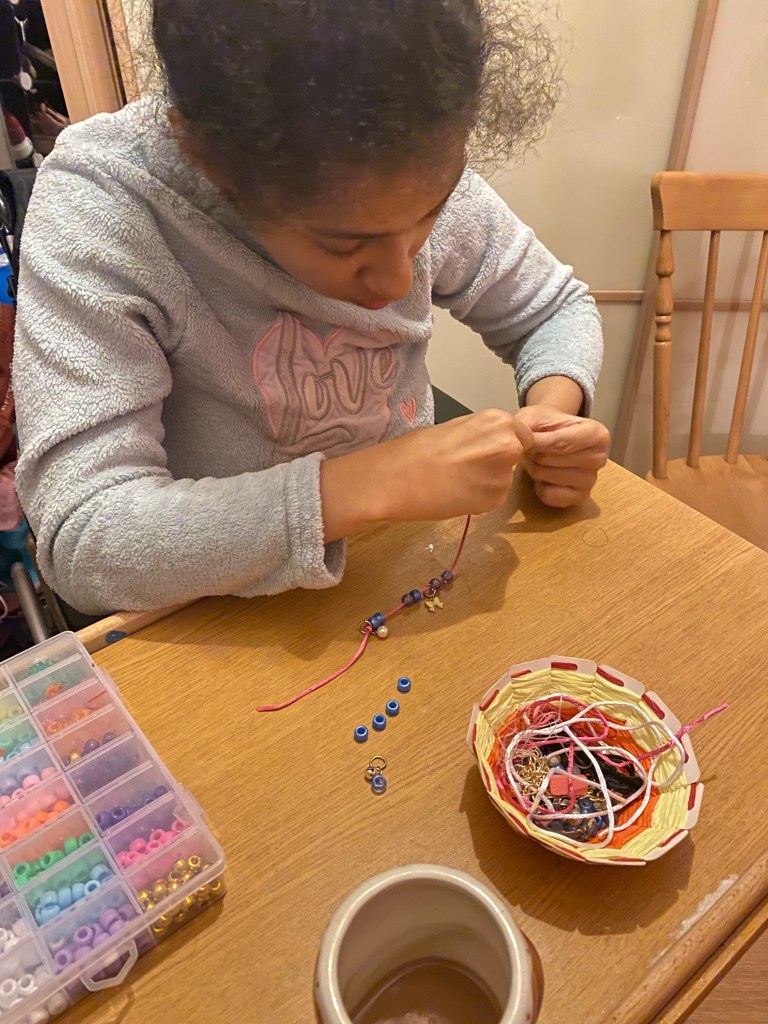Man With MND Invents Gadgets To Help In Daily Life
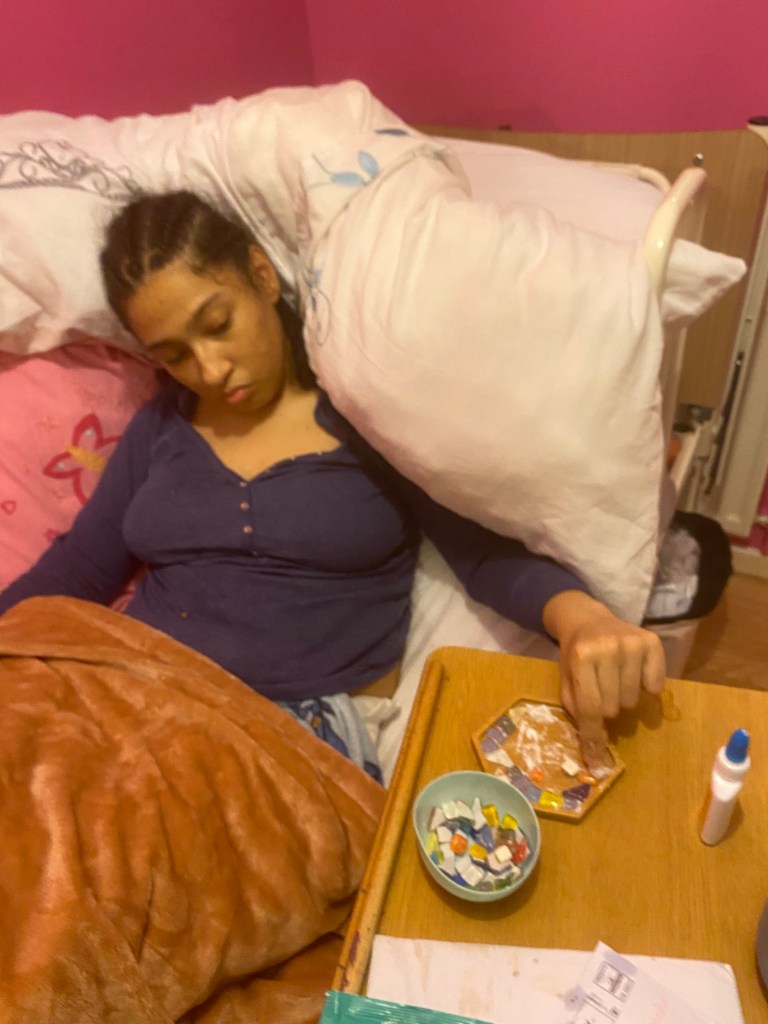
A technology expert who lives with Motor Neurone Disease (MND) has used his skills to create a range of gadgets to make his daily life easier.
Andrew Herbert, 55, from Skipton, was a keen cyclist and runner before being diagnosed four years ago with the condition, which affects nerves found in the brain and spinal cord.
He has since invented tools, including a motorised device which rolls back his bed covers, to help make himself more independent.
Andrew, who works as chief technology officer at a Leeds-based finance firm, said he now had had “over 100 sensors in the house” which allowed him to control domestic appliances.
MND leads to the weakening and stiffening of nerves over time and usually affects how sufferers walk, talk, eat and breathe.
Progression of the disease can be rapid – with more than half of those affected dying within two years of being diagnosed.
It is a relatively rare condition most common in people over 50, but adults of any age can be affected.
About 5,000 adults in the UK have the disease at any one time.
Andrew said of his MND diagnosis that it was “quite a shock at the time, because I’ve always looked after myself”.
“It was quite devastating for my family, too, because of the known outcome and what potentially I would have to go through and how they would be affected by that,” he said.
Andrew’s wife, Nicola Herbert, said her husband’s technological know-how had given him a greater degree of independence than he might otherwise have had, given his condition.
She said: “It’s just inspirational, really, how brave he’s been and how he’s put his time to really purposeful pursuits rather than whiling away the time.
“He’s just so inventive and positive all the time.”
The gadgets devised by Andrew have meant the workload for care staff has also been lightened.
Carer Lauren Sykes said: “Andrew switches between the laptop, the computer and his phone.
“If he wasn’t doing that, I’d be doing a lot of tasks for him, but he just does things by himself.
“So that saves a lot of time and I can be off doing something else, while he’s working.”
Andrew said he was deploying technology to make life a little more comfortable, not just for him but to inspire others who were in a similar situation.
Such is his enthusiasm for tech-savvy solutions, that he has shared his tips on social media.
“I think it’s really important to have purpose in your life and the technology that I invent and the work that I do gives me that,” he explained.
Decorating glass jars project with acrylic pens
Bowling with one of my activity groups
Instagram Investigating AI Profiles ‘Fetishising’ Disabled People
Instagram’s parent company, Meta, is investigating AI-generated social media accounts that sexualise disabled people appearing on its platform.
It comes after the BBC flagged dozens of profiles showing AI-generated images of women with disabilities, including Down’s syndrome or vitiligo.
Some profiles post fake images and videos of women with missing limbs, visible scarring or in wheelchairs. Many are in sexualised positions, wearing revealing clothing.
Some accounts have amassed hundreds of thousands of followers in a matter of months. One profile, claiming to be conjoined twins, has about 400,000 followers, despite only joining Instagram in December 2025.
Kamran Mallick, chief executive of Disability Rights UK, said the emergence of “accounts that fetishise, mock, or monetise the identities of disabled people is nothing short of horrific”.
He added: “What we have here is technology weaponised to strip disabled people of their agency and dignity, turning our lived experiences into digital caricatures for the profit and titillation of others.”
Medical charities have also voiced concern. A spokesperson for Gemini Untwined, which funds specialist surgery for rare newborns joined by the head, said portraying conjoined twins as entertainment was “morally reprehensible”.
They added: “We witness first-hand the medical challenges that these children and their families endure, which makes the portrayal of conjoined twins as a form of entertainment or spectacle especially problematic.”
Dr Amy Gaeta, from the University of Cambridge, told the BBC she researches how AI shifts power in relation to gender and disability. She said the internet is “flooded” with free and low-cost generative AI image-making tools.
Generative AI is a type of software that creates new content based on patterns it has learned from existing data in response to a user’s prompt.
Gaeta said while some tools have restrictions on content, like banning sexually explicit prompts, others do not or can be easily bypassed.
“Sometimes, without my prompting or intent, hypersexualized images of disabled people will be generated. This clearly shows a bias in the datasets that these tools are trained upon,” she said.
An Ofcom spokesperson said it was “tracking how AI is evolving, the risks that may emerge, and what actions may be needed to address them”.
They said the watchdog’s online safety rules require tech firms to tackle illegal content and protect children from harmful material – including abusive or hateful content.
The Online Safety Act requires platforms like Instagram to apply terms of service consistently, including where content mocks people based on protected characteristics, like their disability.
The Equality and Human Rights Commission said the accounts flagged by the BBC were “deeply disturbing”, adding: “It’s vital there are robust regulatory powers in the digital space to protect people from harm.”
A spokesperson for Meta said it was investigating the content and that it removes material that promotes sexual exploitation or attacks people based on protected characteristics.
While these accounts are generating fake personas, there is serious concern over the commands for the generative tools behind them.
Alison Kerry, head of communications at disability equality charity Scope, said the practice amounted to “discrimination dressed up as content”.
She added: “These AI images don’t appear from nowhere – they’re built from real disabled people’s images, often without consent – and unmoderated comment threads turbocharge objectification and harassment.”
Gaeta said moderation on sites like Instagram is not strong enough.
“Even when safeguards are in place, it has been proven relatively easy to bypass these if someone is insistent enough on doing so,” she said.
“Big tech needs to be held accountable just as much as misogyny and ableism need to be tackled.”
Tourette’s Campaigner Says BBC ‘Should Have Worked Harder’ To Stop His Slur Being Aired
Tourette’s campaigner John Davidson has said the BBC should have “worked harder to prevent anything that I said” at the Bafta Film Awards being broadcast, and questioned why he was seated near a microphone.
Davidson, whose condition involves involuntary tics, shouted a racist slur while black actors Michael B Jordan and Delroy Lindo were on stage at Sunday’s ceremony.
Davidson told Variety, external: “I remember there was a microphone just in front of me, and with hindsight I have to question whether this was wise, so close to where I was seated, knowing I would tic.”
The BBC reiterated that the offensive language “arose from involuntary verbal tics associated with Tourette syndrome”, adding: “We apologise that this was not edited out prior to broadcast and it has been removed from BBC iPlayer.”
On Tuesday, the corporation’s chief content officer Kate Phillips told staff that another racial slur had been edited out of the broadcast.
In contrast, the one shouted when Lindo and Jordan were on stage “was aired in error and we would never have knowingly allowed this to be broadcast”, she said.
Davidson, from Galashiels in Scotland, said he shouted about 10 different offensive words during Sunday’s ceremony as a result of his tics, but the media coverage has given the impression the N-word was the only one.
Variety reported that he has contacted Warner Bros in order to apologise directly to Jordan, Lindo and Sinners production designer Hannah Beachler, who also spoke about hearing racial slurs.
Meanwhile, Google has apologised after sending a news alert, external about the story which included the N-word.
“We’re very sorry for this mistake,” the company said of the computer-generated alert. “We’ve removed the offensive notification and are working to prevent this from happening again.”
Davidson told Variety that the studio behind the film I Swear, which tells the story of his struggles with Tourette’s, held discussions with Bafta before the ceremony about the possibility of his ticking.
“StudioCanal were working closely with Bafta, and Bafta had made us all aware that any swearing would be edited out of the broadcast,” he said.
“I have made four documentaries with the BBC in the past, and feel that they should have been aware of what to expect from Tourette’s and worked harder to prevent anything that I said – which, after all, was some 40 rows back from the stage – from being included in the broadcast.”
‘Comprehensive review’
Awards ceremonies often have microphones placed at various spots around the auditorium, to pick up ambient crowd noise as well as applause and cheering.
In a statement on Monday, Bafta said it acknowledged the “harm this has caused, address what happened and apologise to all”.
In a letter to its members on Tuesday, the organisation said it wanted to “assure all our members that a comprehensive review is under way”.
After shouting the slur, Davidson said he chose to leave the auditorium “so as not to cause any more upset”, adding that Bafta found him a private room with a monitor to watch the rest of the ceremony.
Davidson said he “had as much right to attend as anyone”, as the subject and executive producer of I Swear, which was nominated for five awards.
“I also knew that as voting members, most people in the audience would have seen I Swear and would be well prepared, well educated and well informed about my condition,” he said.
Davidson said he was “aware of how physically and mentally difficult it would be for me to attend”, adding: “I can’t begin to explain how upset and distraught I have been as the impact from Sunday sinks in.”
‘The opposite of what I believe’
In his interview with Variety, Davidson also said: “I want to be really clear that the intent behind them [the tics] is zero. What you’re hearing is a symptom – not my character, not my thought, not my belief.”
He said he felt a “wave of shame an embarrassment” after shouting the racial slur.
“Tourette’s can feel spiteful and searches out the most upsetting tic for me personally and for those around me,” he explained. “What you hear me shouting is literally the last thing in the world I believe; it is the opposite of what I believe.
“The most offensive word that I ticked at the ceremony, for example, is a word I would never use and would completely condemn if I did not have Tourette’s.”
Several figures in the Tourette’s community have also sought to explain the condition.
Writing on Instagram,, external Baylen Dupree, star of US reality series Baylen Out Loud, explained: “Tourette’s doesn’t pull from hatred – it often pulls from anxiety, from fear, from the very thing you’re most scared of saying.
“The brain misfires on what feels charged or taboo. It doesn’t excuse the hurt a word carries. Words matter. History matters. Pain matters. But so does neurological reality.”
BBC News understands the producers editing the ceremony for its delayed BBC broadcast were doing so from a TV truck and simply did not hear the slur shouted when Lindo and Jordan were on stage.
But Channel 4’s former head of news and current affairs, Dorothy Byrne, rejected that defence in an interview with BBC Radio 4’s Today programme on Wednesday.
“John needed a BBC person next to him at all times to support him, but also to relay and be aware of anything that he said,” Byrne reflected.
“So there needed to be, in the written plan, a means by which the people in the truck would be aware of what happened in the room.”
‘Deeply traumatising’
Former BBC News executive and Conservative communications chief Sir Craig Oliver said the TV truck defence was “kind of entering into the dog-ate-my-homework territory”.
“It’s increasingly obvious that we live in a time where there are going to be controversial things at live events, and there is going to be potential reputational damage to the BBC,” he said.
“So does it have that grip, does it have that process in place? And increasingly it seems like the answer is no.”
Meanwhile, BBC Radio 1 DJ Oré Olukoga has expressed his disappointment with how the situation has been handled by the corporation.
Olukoga, the station’s early weekend breakfast host, wrote on X, external that the “incident at the Baftas and the reaction to it has been deeply traumatising”.
“I understand all the nuances at play and would never want to minimise someone’s plight, but as a Black man who works for the BBC, I am deeply, deeply disappointed in how it’s been handled,” he said.
A Quick Thanks To Eastenders
This is a quick and short post to thank Eastenders for their recent coverage of three very important disability issues at different stages of life.
- Nugget’s epilepsy, caused by a tragic event, just beginning in his teenage years.
- Penny’s pregnancy, thankfully the result of a ‘normal’ romantic relationship (is there any such thing?). Sadly Jack initially reacted with concern related to her disability but thankfully he now seems to have changed his mind.
- Nigel’s dementia, in older age, which will eventually lead to his life ending.
Eastenders have made this disabled viewer feel very happy, included, wanted and welcomed in recent months. They deserve thanks and I look forward to seeing how all three storylines play out.
My respite care will not be funded by social care, who would like me to go to a respite care home instead. A care home is an inadequate solution for the disability I live with- functional neurological disorder, as well as, cerebral palsy. I have tried it in the past and instead of giving me and my family a break, it had a terrible impact on my mental health. That meant my family was even more stressed. It is mentally destroying to go there because there are people with severe disabilities who cannot communicate at all. This feels like a punishment and mentally I can’t cope in that environment. It also makes my FND worse. Social care told me they’d never fund a personal budget for my respite care/ direct payment, which I have for the rest of my support. They continue refusing to put my respite care element in my direct payment/personal budget package. They will only pay for me to go to a respite care home of their choice and brokerage are saying I do not have a say in this; and that they will find one that says they can meet my needs. I do not see how they will do that, as there is no training for FND that I can even send my own staff on. My own staff on the other hand know me well and know how and when to call my doctor and nurses.
The ‘Brilliant Invention’ Helping Cancer Patients
When Tim Morgan was diagnosed with chronic lymphatic leukaemia he started going through radiotherapy – but his treatment hit a roadblock when it triggered his claustrophobia.
The 63 year-old from Telford was being treated at the Royal Shrewsbury Hospital, and the radiotherapy involved a thermoplastic mesh mask moulded to fit the shape of his head and neck. He managed to go through the first two doses but needed a further 10.
“I had a panic attack, I couldn’t do it. The holes are just so tight, I had to stop halfway though,” he said.
He wanted to complete the treatment instead of going on to chemotherapy. That is when he was told that there was a new mask that could help.
Lingen Davies Cancer Support, which helps people living with the disease in Shropshire, Telford and Wrekin and Mid Wales, has funded surface guided radiotherapy technology (SGRT) on two radiation machines at the Royal Shrewsbury Hospital.
This allows patients to receive radiology with an open-face mask and is something not widely available on the NHS.
“You can see, you can open your eyes, you can breathe through your nose and your mouth,” Morgan said.
“The full face mask, you can’t even open your lips. I still found it slightly claustrophobic but towards the end I got quite used to it.”
With the new mask, staff also helped Morgan with breathing exercises.
He said the mask had made a real difference, since his claustrophobia is something he has suffered with since he was a child.
“It’s a brilliant, brilliant invention, I wouldn’t be able to do it otherwise,” he said.
“The panic attack I had, I just could not go ahead with it, but this other one it makes it so much easier.”
“In the future as we develop this service, more patients who would ordinarily refuse treatment or require sedation can instead be offered an alternative option,” said Amanda Welsh, chief dosimetrist at the hospital.
“Who knows where this cutting-edge technology will take us in the future.”
Naomi Atkin, CEO of Lingen Davies, added: “This technology has completely transformed the experiences of those in our region receiving radiotherapy treatment.
“Hearing Tim’s lived experience highlights the huge difference SGRT has made for those facing cancer treatment.
“SGRT is not yet widely offered in NHS Trusts but we want to ensure people across Shropshire, Telford and Wrekin, and Mid Wales have access to its wide-ranging benefits, including reduced treatment and waiting times as well as improved wellbeing and quality of life.”
Hold My Hand- UK’s First BSL Dating Show
A contestant on the UK’s first British Sign Language (BSL) dating show says he hopes it teaches people about the deaf community – and shows they can “have banter” too.
Oliver Scott is among the first to take part in the new series, Hold My Hand, which follows deaf or children of deaf adult (CODA) contestants as they navigate dating through BSL.
The 27-year-old from Norwich tells BBC Newsbeat, through an interpreter, the show felt “refreshing” after always questioning “why couldn’t I be a contestant on something like that” when watching other dating shows.
It is the latest from LumoTV, a deaf-led streaming platform, and is presented by deaf identical twins Hermon and Heroda Berhane.
Created with the deaf and signing community, the three-part series aims to highlight deaf culture and identity in a way that isn’t widely seen on screen.
Oliver grew up in a deaf family where BSL was his first language so he “didn’t feel the need” to get a hearing aid or a cochlear implant.
He says he often thought about what it would be like to be on a TV show, but worried about how it would work.
“We’d say it’s impossible because of the communication, everybody talking, the different games are quite fast-paced, the gossip, the drama,” he explains.
“How would I get to know people? It might be quite difficult.”
However, he says he had a “fantastic experience” on Hold My Hand and felt he could “genuinely get to know a girl better”, while having “a bit of banter”.
Back in 2022, model and dancer Tasha Ghouri became the first deaf contestant on ITV dating show Love Island.
Oliver says Tasha is a “brilliant representative” of somebody that uses a cochlear implant – a small electronic device that helps her to hear – within mainstream media.
However, he feels its important to show that deaf people have different communication preferences.
“They might see Tasha and think she speaks very well and think all deaf people are the same, and that’s not the case,” he says.
“I prefer to use British Sign Language. That is my first language. So I think we need more reflection of British Sign Language users in the mainstream.”
Oliver hopes people can learn more about the deaf community by watching Hold My Hand, and also challenge some misconceptions.
“We can be naughty, we can be mischievous, we can be cheeky, we can have fun, we can have great banter too,” he says.
“It’d be really nice to expose hearing people to that too.”
Across wider media, he feels representation has been improving but he would like to see a deaf BSL user on a “mainstream reality show”.
Teri Devine, associate director of inclusion for the charity Royal National Institute for Deaf People, says Hold My Hand is a “huge milestone” for representation of the deaf community.
“It really matters. Everybody wants to see somebody that’s like themselves,” says Teri.
“So if you see somebody on television that’s a deaf person that’s going on a date, you think: ‘Oh, actually I can do that’.'”
Teri adds that it can also help people find their “role models” which can encourage them to feel like “they can achieve anything they set their minds to”.
The environment in which a date takes place can also make a difference for a deaf person, Teri explains.
She says places which are quieter and brighter so the deaf person can see their date’s face and read their lips can help make navigating dating easier.
There has been increased representation of the deaf community in recent years on television, including actress Rose Ayling-Ellis becoming the first deaf contestant to compete, and win, Strictly Come Dancing in 2021.
Ayling-Ellis also made history when she became the first deaf person to host live sports coverage on TV as one of Channel 4’s hosts for the 2024 Paris Paralympic Games.
– Hold My Hand is available to stream on LumoTV and YouTube
UK Athletics Pleads Guilty To Corporate Manslaughter
UK Athletics has pleaded guilty to the corporate manslaughter of Paralympian Abdullah Hayayei.
Hayayei died aged 36 after a metal cage fell on him while training at Newham Leisure Centre, London in July 2017.
UK Athletics pleaded not guilty to the charge in March 2025 but entered a fresh plea on Friday at an Old Bailey hearing.
Keith Davies, the head of sport for the 2017 World Para-athletics Championships, also pleaded guilty to a health and safety charge, having previously denied gross negligence manslaughter.
Prosecutor Karen Robinson asked the court to set a two-day sentencing hearing in early June, confirming the prosecution would not seek a trial and the outstanding charges would be dealt with at the conclusion of the sentencing.
Davies, 78, was granted continued bail on the condition he liaise with the Probation Service for a pre-sentence report.
Hayayei was training for the World Para-athletics Championships in London at the time of the incident.
The United Arab Emirates thrower had been set to compete in the F34 shot put, discus and javelin events.
Hayayei, a father of five, finished sixth in the javelin and seventh in the shot put when making his Paralympic debut at Rio 2016.
London 2017 was due to be his second appearance at a worlds. At the 2015 event in Doha, Qatar, Hayayei finished fifth in the discus and eighth in the shot put.
A moment of silence was held in honour of Hayayei during the opening ceremony at London Stadium.
Dream Catcher Art Project at the Day Light Club
Blind Gamer’s Two-Hour Live Stream For Charity
Blind gamer Dom Hall attracted thousands of viewers during a two-hour gaming session which he streamed live on two social media platforms.
The 39-year-old had 1,387 viewers and 27,500 likes on TikTok, 120 viewers on Twitch and attracted followers from the UK, USA, Canada and the Netherlands.
Hall also raised more than £300 for the iSightCornwall charity which is celebrating its 170th year.
He said he was nervous because he needed to play Mortal Combat with the sound coming from the game and people asking questions at the same time. “All the sound coming through at once was a bit tricky,” he added.
A tumour in his optic nerve left Hall with only 10% sight when he was three years old and total loss of sight by the age of 35.
Hall has been a keen gamer since he was five, saying he was attracted to the colours and the interaction with other people.
But when he completely lost his sight he thought he would have to stop gaming.
“I thought this is it, there goes the hobby,” he said. “But thankfully I did a bit of research into it and found there are games being made today that are accessible for visually impaired people. You can play games entirely through sound by games that support it.
“This is done by screen readers that read out everything on screen for you or the text, as well as audible cues for visual things in a surround sound headset,” he said.
‘Sight loss journey’
Hall is iSightCornwall’s assistive technology advisor and his colleague Beth Perry helped him with viewers questions on the live stream.
“We see people at all stages of their sight loss journey,” said Perry.
“I’ve seen some people come in absolutely convinced there’ll never do something again, something they used to really, really love.
“They have an hour appointment with Dom and they come out and they’re almost excited to go home and try it a different way,” she said.
Peppa Pig Hearing Loss Story May ‘Remove Stigma’
An upcoming Peppa Pig episode in which George gets a hearing aid could help to “remove some stigma” around hearing loss, the head teacher of a prominent school for deaf children said.
Peppa’s brother receives the device for partial hearing loss in the upcoming storyline from an audiologist voiced by Gladiators star Fury.
The episode has been developed in partnership with the National Deaf Children’s Society and is due to come out on 9 March.
Paul Burrows, head teacher at the Royal School for the Deaf in Derby, said the story was “very important” in helping deaf children “not feel so different”.
Burrows said: “I am not quite sure [I would use] the word normalised but what it is doing is making having a hearing aid, going to the audiologist… just part of life and I think having as much representation as you can of that is fantastic.
“It is very important for them [the students] themselves, it allows them to not feel so different, it might kind of remove some stigma.
“But I think actually for me the importance of this will be wider than the deaf young person.
“I think it will be for their brothers and sisters, their families, their friends, the people they go to school with because they will all see it.”
Burrows said the school taught their students to be “proud of their deafness” and emphasised the “solution is not always just – ‘let’s get a hearing aid'”.
“We are big supporters of British Sign Language (BSL) for example as a way of communicating,” he said.
“So the technology is one side of it but I think equally we need to teach people that being deaf is just a part of who they are, there is nothing wrong with you if you are deaf, that’s just you – it’s part of your makeup.”
George’s audiologist is voiced by Jodie Ounsley, also known as Fury from Gladiators, who uses a cochlear implant.
The former England rugby union international said she sometimes felt “lonely” growing up as she was “probably” the only deaf person in her school.
She said: “I can just imagine if I had something like that when I was younger and saw it on TV… just normalising it, I think that would have had a huge impact on me.”
The school in Derby was founded by Dr William Roe in the 1890s after witnessing a young deaf man being bullied.
Roe was “struck by the social and educational exclusion of deaf people” and so set out on a world wide tour to raise awareness and funds, the school said.
It currently accepts students aged three to 19.
Patients Describe ‘Culture Of Abuse’ As 15 Hospital Staff Arrested
Patients, relatives and whistleblowers have described a culture of abuse at a mental health hospital, while 15 staff members have been arrested following allegations of rape, ill-treatment and neglect.
St Andrew’s Healthcare in Northampton, which provides specialist care for about 600 people with complex mental health needs, is the subject of three police investigations following alleged assaults and the deaths of two patients.
The charity that runs the private hospital said it had dismissed several staff members and was delivering an urgent action plan to address the issues.
St Andrew’s Healthcare said it was committed to “full transparency” and took a “zero-tolerance approach to any allegation of harm or poor practice”.
The Care Quality Commission (CQC) rated the hospital as inadequate last year and imposed an urgent condition on its registration, and new admissions have been restricted.
Warning: This article contains distressing content
Anne, whose name has been changed, told the BBC she was horrified by the injuries sustained by her daughter while she was a patient at St Andrew’s Healthcare.
“They were restraining her with four adults and on one occasion she was knelt on by a male member of staff,” she said.
“She was waking up every night for months and was obviously in a severe amount of pain with her ribs,” she added.
Anne said her daughter had “lost half her body weight” and showed “all the symptoms of being malnourished”.
“She lost the use of her hand while in long-term segregation” and on two occasions she had suffered severe burns from coffee, she added.
Anne has made a series of safeguarding referrals to West Northamptonshire Council, but said she had not gone to the police due to the lack of witnesses and CCTV.
“It’s traumatic. Something’s got to change and the only way things can change is by people now speaking out,” Anne said.
Northamptonshire Police said 15 people had been arrested as part of investigations into incidents at the hospital that reportedly took place since October 2024. Ten people remain under suspicion and have been bailed or released pending inquiries.
- Eight people were arrested on suspicion of wilful neglect and ill-treatment in relation to an alleged assault in July 2025 on a man with a brain injury. One person was also arrested on suspicion of rape. All remain on bail
- Five people were arrested on suspicion of corporate manslaughter and gross negligence manslaughter following the death of a man in February 2025. Four face no further action while one person remains on bail for the offence of wilful neglect by a care worker
- One woman was arrested on suspicion of assault and ill-treatment or wilful neglect following an incident on 29 June 2025 and remains on bail
- One person was arrested in relation to an investigation into gross negligence manslaughter following the death of a teenage girl in October 2024. Police said no further action would be taken
‘Horrendous injuries’
Jamie, whose name has been changed, was a staff member at St Andrew’s Healthcare until recently and has spoken out about “massive safeguarding issues” at the hospital.
“I’ve seen senior nurses goading a patient,” he said.
He added that a patient who was being observed on a one-to-one basis by staff had incurred “horrendous injuries” after self-harming when staff were withdrawn.
On another occasion, Jamie said he had been locked in a room with an “extremely violent” patient after a nurse refused to open the door.
He also described bed-bound patients being ignored while screaming in distress and others being roughly handled.
“When you do restraints, you’re supposed to do them in a certain way, and some patients were getting pulled to the floor by their arms – that’s not restraint,” he said.
He claimed that instances of what he considered “cruelty and neglect” were due to poor culture and unqualified staff who “didn’t have enough experience”.
An employee, who wanted to remain anonymous, told the BBC they were now “ashamed” to work at St Andrew’s Healthcare.
“It is so sad, some staff trusted to work with patients have acted so terribly. Not all staff are bad, but the organisation needs to take action to make sure patients are protected,” they said.
‘My wrists popped’
Beth Sheridan, 26, from Northampton, was a patient at St Andrew’s Healthcare in 2021 and said staff would “fall asleep quite a lot – at one point I managed to do something to myself where I needed CPR because one of them was asleep”.
“[Staff would] bend people’s arms back, be dragging them across the floor,” she said.
Sheridan said staff once came to restrain her after an emergency alarm had been pulled and “they bent my wrists back and one of my wrists popped”.
She continued: “I was screaming out saying that it was hurting. Nobody cared. Nobody told them to stop. No-one told them it was wrong.”
The charity’s services are largely commissioned by the NHS and it had an income of almost £220m in the year ending March 2024.
During an executive meeting, recorded and leaked by a staff member, Sanjith Kamath, the hospital’s medical director, said the charity may not be able to continue in its current state of “significant financial stress”.
However, St Andrew’s Healthcare said in a statement that the hospital was being reshaped “to be a smaller, more focused charity”.
“In the year ending March 2025, we made a small surplus, giving us the resilience to navigate the financial challenges we currently face,” it said.
St Andrew’s Healthcare said it had reported the cases subject to Northamptonshire Police investigations to the force and launched internal investigations.
“All staff were immediately suspended and several staff were dismissed. We referred several members of staff to the Nursing and Midwifery Council,” the spokesman said.
The hospital said the use of restraint was carefully planned and only undertaken as a last resort, but it acknowledged “care hadn’t always met the standards patients deserve” and apologised to those affected.
It added it had introduced new training for all front-line staff, had significantly reduced the use of agency staff and had now installed CCTV on most wards.
Blind Couple Say Sight Loss Is No Barrier To Love
A blind couple from Scarborough have said they hope the story of their upcoming marriage can inspire other visually impaired people who are nervous about dating.
Malcolm Day and Sarah Brooks are due to tie the knot in September after meeting on holiday in Blackpool in June 2024.
They will marry a year to the day since Sarah, who became visually impaired in 2016, made the 260-mile (418km) trip from Winchester in Hampshire to the North Yorkshire coast to live with Malcolm.
Sarah said: “I was calling it love at first sight and trying to do everything to make sure Malcolm felt the same, but I didn’t have to work that hard.”
The pair originally met at an event attended by 80 visually impaired people at a hotel in Blackpool, according to Malcolm, who has been blind since he was 14.
“I knew two or three people in the group. They’d invited me along and said, ‘come and have a good time. You’ll meet some new people’,” he explained.
“I never intended meeting someone like Sarah.”
Malcolm said he proposed to Sarah during a karaoke night in June last year when they returned to the seaside resort for another holiday a year after they first met.
“We’d decided we were going to do Sonny and Cher’s I Got You Babe,” he said.
“I completely messed it up because my mind was somewhere else. I was distracted by thinking, ‘I’ve got this ring in my pocket’.
“There’s a line in the song that says, ‘she wears my ring’. So when I got down on one knee I said, ‘there’s something in that song I’m going to put right’.
Remembering that moment, Sarah said: “I didn’t know at all, I didn’t see it coming.”
In September, the couple bought a house together in Scarborough, where Malcolm is originally from, and that is where they live now with their three dogs.
“In the last three or four months, we’ve been discovering each other’s eyesight as two blind people,” Malcolm said.
“I’ve learned a lot about what Sarah can see, and Sarah has learned a lot about what I can see.
“We joke to people that we have one good eye between us.”
Sarah said that for their wedding in September, her bridesmaids would all be visually impaired.
“My friends, my lovely, lovely blind girlfriends – nine of them – will be on the bridesmaid list,” she said.
“Mostly, it’s a big blind community getting together.”
Irena Valchera, who is visually impaired and works for social inclusion charity Eye Matter, and who will also be one of Sarah’s nine bridesmaids, said many of the organisation’s members had found dating a tough challenge.
“It must be very difficult to overcome that shyness or thinking, ‘maybe I am not good enough’,” she said.
“It must be very scary and isolating.
“We have in Eye Matter young people who I know are suffering because of that.”
However, Malcolm and Sarah said they wanted their successful relationship to inspire other blind people who were nervous about meeting new people.
“Everybody has something that holds them back. Sight loss doesn’t have to be that thing,” said Sarah.
“We can still get out there. We can still do it. We can still go on a blind date.”
It’s nearly 200 years since the birth of a British aristocrat who became the first Muslim member of the House of Lords.
But few have heard of Lord Henry Stanley, who “defied convention and his family’s wishes” when he converted to Islam in 1859, according to historian Jamie Gilham.
Little remains of Stanley’s letters and diaries “which is really frustrating but adds to the idea that he was a private man,” he said.
Since medieval times, a relatively small number of Brits had become Muslims while travelling abroad.
But Gilham said Stanley was notable as he had influence politically and on his lands in Cheshire and Anglesey.
Born in 1827, Stanley was the eldest of 10 children given free rein to develop their own thoughts and beliefs.
The wider family, whose aristocratic ancestors can be traced to Norman times, had members belonging to various Christian denominations and at least one who was Jewish during Victorian times.
Family historian Lady Carla Stanley, who is married to the current Lord Stanley, said they were “free thinking” and born to educated, well-travelled mothers.
“They were people who did things,” she added. “It was acceptable to be argumentative.
“Thinking, debate, discussions were OK as opposed to a ‘get off my land, I’m going shooting’ attitude.”
Like many educated Victorians, Stanley was dazzled as a child by travelogues and the Arabian Nights tales.
He also had a hearing impairment which affected his schooling, and he left Eton after one year to study with a private tutor.
Gilham said Stanley’s father, who was an MP, and his mother – who helped establish the first women’s college at Cambridge University – had “great expectations for their first-born”.
However his struggles with hearing meant “his family worried greatly about his future prospects”.
“He only really started to shine when he went to Cambridge and learned Arabic,” Gilham added.
Within a year, the 20-year-old was employed as an assistant to the then Foreign Secretary, Lord Palmerston in 1847.
Over the following decade, Stanley worked for the diplomatic service, with postings in the Turkish-based Ottoman Empire, as well as Greece and Bulgaria.
“Stanley came to appreciate the social and the spiritual benefits Islam provided the Ottomans,” Gilham said.
It was also a time when various European empires were reaching their peak yet faced republican or nationalistic revolts.
“From letters, we see that Stanley experienced both political and spiritual crises,” Gilham added.
“He didn’t lose faith in God but he certainly had theological doubts. He did question the literal accuracy of the Bible, for example, and the letters between his parents show that he didn’t go to church for the first time in his life.
“Unusually for Britain in the mid-Victorian period, Stanley did gravitate towards Islam – the religion of the Ottoman Turks – and symbolically at that time, around 1849-50, he gave up wine.”
Disillusioned with Britain’s expanding imperialism, Stanley quit the diplomatic service in 1858 and decided to become a Muslim some months later while travelling in Arabia.
“There’s little account of his religious conversion and beliefs,” Gilham said. “It’s just things that you can read in some of the family letters.”
Press reports of Stanley’s conversion emerged in Sri Lanka on his visit there in 1859, before news travelled back home to Cheshire – where it was reported in the local Macclesfield Courier and then the national outlets in London.
Some reported that he made a pilgrimage to Islam’s holiest site in Mecca and adopted the name Abdul Rahman – Arabic for “servant of the merciful Lord” – although evidence is unclear, Gilham added.
“Letters show his parents were absolutely furious and equally embarrassed and humiliated that their son would convert to Islam from Christianity.
“His father said to his mother, ‘Is he mad? What can he possibly mean by parading himself in our colonies and our possessions in the degrading position he occupies?’
“His mother replied to his father that the newspaper report in the Macclesfield Courier ‘made me feel sick’.”
They later issued a public denial that their son had converted to Islam however Stanley wrote to one of his brothers that “I have always been a Mussulman [Muslim] at heart”.
Secret wedding
In 1862, he married a Spanish Catholic lady in Algeria under Islamic law, but kept their relationship secret until his father’s death seven years later.
It emerged his wife was already legally married to a Spanish man at the time of their wedding, although it’s unclear if Stanley was aware of this, Gilham said.
The couple registered their marriage under English law after he became the third Lord Stanley of Alderley and second Baron Eddisbury on his father’s death in 1869.
“The Spanish husband was still alive until 1870 so again, the marriage wasn’t actually valid.
“But it was eventually made valid when they remarried in 1874 and that was a Roman Catholic ceremony, which kind of raised eyebrows,” Gilham explained.
“I think he was respecting the religion of his partner, his wife.”
Pub closures
After inheriting his father’s lands and titles, he took his place as a non-partisan crossbench peer in the House of Lords in 1869 and became its first Muslim member.
“I don’t know how many of his peers would have known that he was a Muslim,” Gilham said.
“I guess they would have because they read the newspapers and knew he was involved in Orientalist societies.”
Lord Stanley inherited lands in north Cheshire, including the village of Alderley Edge – better known as an affluent area near Manchester that’s popular with Premier League footballers.
“Famously or infamously, he did close some of the public houses on the Alderley Park estate,” Gilham added.
Following the death of an uncle in 1884, Lord Stanley inherited the Penrhos estate in Anglesey, north Wales, where he contributed to the upkeep of local churches.
He also paid for windows with geometric designs rather than traditional figurative scenes, in line with Islamic rulings against the drawings of creatures.
“As a Muslim, Stanley respected Christianity as a sister faith of Islam – of its shared Abrahamic roots,” Gilham said.
Eve Hawwa Iqbal-Khokhar, an English woman who converted to Islam and volunteers in the Manchester Muslim community, said she “felt compelled to visit” the churches after finding out about Lord Stanley’s life just before a family holiday to Anglesey.
“History really excites me and learning about the first converts to Islam in Victorian Britain is so exciting – especially a local aristocrat of Lord Stanley’s standing.”
She described the churches’ designs as a “visual feast”, adding they form part of “a rich tapestry of our past”.
However as a supporter of the political union of the UK nations, Lord Stanley disapproved of teaching Welsh in local schools.
“He really respected language,” Gilham said. “But I guess in this case it was about the union and the union was more important to him.”
He described Lord Stanley as someone who “didn’t believe in the extension of empire”, adding: “He believed in the consolidation of the empire as it was.
“And so he spoke out in the Lords about preserving the empire, but also about looking after its people.
“He was a conservative man but also a Victorian. He did defy convention in many respects – and a crucial respect in terms of religion – but in other ways he didn’t.”
Lord Stanley died at the age of 76 during the Islamic holy month of Ramadan in 1903 and was buried in unconsecrated ground on his Alderley estate, in a service led by an imam from the Ottoman Embassy in London.
“In some respects he was ahead of his time and he is starting slowly to be recognised and reclaimed to some extent,” said Gilham.
“He was not showy and maybe that was to the detriment of his legacy but I hope people will start to recognise him a little more than maybe he has been so far.”
Having my make up done for my first night out of 2026
Stay tuned in for my respite break content! Coming up in the next few weeks, but here is how my PA enable my independence, enabling me to go on the night out, helping me to get ready and present myself the way I would like to.
My pyjama day/weekend
CP Healthcare Is A Never Ending Battle For Adults
https://www.bbc.co.uk/news/articles/cjwz3xl2gevo
A woman with cerebral palsy says guaranteed annual health checks for people with her condition could end “fragmented” health care.
Adults with cerebral palsy risk developing early-onset health conditions like chronic pain, mobility difficulties and cardiovascular disease.
Molly Lane, who lives in Salisbury in Wiltshire, said: “You spend your life navigating a fragmented [health] system. For some people, it’s a never-ending battle.”
A spokesperson for the Department of Health and Social Care (DHSC) said the government was “strengthening care for people with complex long-term conditions, including cerebral palsy” through its 10 Year Health Plan.
This includes shifting more healthcare to the community by bolstering GP and pharmacist services.
Cerebral palsy is a developmental disability which impacts movement and co-ordination.
It affects about 130,000 adults in the UK, yet routine health checks are not guaranteed.
Lane, 29, decided to share her story after seeing an Instagram post by comedian Rosie Jones, who also has cerebral palsy, sharing the Doctor Won’t See Us Now campaign.
It is calling for annual health checks so people with the condition can avoid long hospital or GP waiting lists when they are already struggling with their health.
After being diagnosed age two, Lane said as a child she received really “brilliant” care from the NHS, including offers of physio and occupational therapy.
But when she reached 19, she said this level of support dwindled and she faced long waits for basic support. It was not until a flare-up at 25 where she realised how little care she had had as an adult with cerebral palsy.
“Everything kicked in and I got referred back to all the specialists I needed,” she said. “From that point, I realised what I missed.”
Lane added: “Adults with cerebral palsy are 14 times more likely to die from respiratory conditions. If you are constantly ill, it can be hard to have the energy to bring issues forward.
“A lot of people with disabilities are taught not to raise their voice, not to be demanding. But never be afraid of complaining or going through the processes. All this campaign is asking for is GP health checks.”
Emma Livingstone, Co-founder and CEO of UP – The Adult Movement for Cerebral Palsy, which is running the campaign, added: “Preventive healthcare is crucial to reducing unnecessary hospital admissions and ensuring a better quality of life for people with CP.”
The DHSC said, as well as the 10 Year Health Plan, Integrated Care Boards across the country were working to provide tailored support for adults with cerebral palsy.
A spokesperson added: “We are committed to ensuring that people with cerebral palsy get the support they need to lead fulfilling, healthy and productive lives.”
Teen Had To Tell Deaf Mum Her Dad Might Die
https://www.bbc.co.uk/news/articles/c5yk9qkwed4o
Hospital staff asked a teenage boy to tell his deaf mother that her father might die, according to the findings of an ombudsman.
The Parliamentary and Health Service Ombudsman said University Hospitals Birmingham (UHB) NHS Trust failed to follow national guidance, by repeatedly using children to interpret critical medical information for their deaf family members.
Alan Graham, who was born deaf and used British Sign Language (BSL) as his first language, died in September 2021 after being treated at the Queen Elizabeth Hospital.
His daughter, Jennifer Petty, who is also deaf, complained about her father’s care. The NHS trust apologised adding “we did not get things right”.
The 52-year-old also raised the issue of hospital staff using her children as interpreters.
The investigation by the ombudsman found the concerns she raised caused significant distress and affected the family’s ability to grieve.
investigates complaints about government departments, other public organisations and the NHS in England.
Their inquiry discovered clinicians asked Petty’s son, who was 16 at the time, to explain that his grandfather might not survive the night and CPR should not be attempted if his condition worsened.
The 75-year-old died the following day.
During an 11-week period in hospital, professional BSL interpreters were provided on only three occasions, the ombudsman found.
Instead staff regularly relied on Petty’s son and daughter, who was 12, to translate complex medical information, including details about the 75-year-old’s condition.
The 52-year-old said the situation was deeply upsetting for the whole family and it was “totally unacceptable” that her children were placed in the position of delivering bad news about their grandfather’s condition.
“My children just wanted to visit their grandad and be there for him as family members but they were constantly being asked to translate by the staff,” she said.
“Having to deliver the bad news about my dad’s prognosis was extremely upsetting for all of us.”
The ombudsman said the trust did not consistently make reasonable adjustments for a deaf patient and his family, despite clear requirements set out in national guidance.
Worry and stress
Rebecca Hilsenrath KC, chief executive of the ombudsman, said public services must be accessible to everyone.
She said deaf patients and their families should not face extra barriers when getting healthcare.
By failing to provide BSL interpreters consistently, the trust caused unnecessary distress in the weeks before Graham’s death, she added, and NHS leaders needed to learn from the case.
The former furniture maker and keen fisherman, originally from Dundee, had moved to Birmingham to be closer to his grandchildren.
He was first admitted to hospital in June 2021 following a fall and was diagnosed with heart failure.
A spokesperson for UHB said: “We offer our sincere apologies to [the family] for their experience, at what was a very difficult time for them.
But, after being discharged in August, he was readmitted with similar symptoms and died two weeks later.
The ombudsman found that the lack of interpreters did not affect the medical treatment he received but did cause worry and stress to his family and limited his daughter’s ability to communicate with clinicians.
The trust was told to draw up an action plan, apologise to the family and make compensation payments of £900 to each grandchild and £750 to their mum.
“We recognise that we did not get things right and understand the impact this had on them.”
Since 2021, actions have been introduced to help deaf patients, including strengthening awareness and accessibility arrangements to ensure patients’ communication needs are better met, they added.
Deaf Patients Condemn Lack Of NHS Interpreters
https://www.bbc.co.uk/news/articles/cx201vrpnx7o
Deaf people say a shortage of interpreters working with the NHS has left them feeling misunderstood, frustrated and facing delays to treatment.
Millie Neadley, 22, from Hull, said she had a “frustrating” year-long wait for surgery on a broken nose after appointments were cancelled because a British Sign Language (BSL) interpreter was not available.
A survey by hearing loss charities RNID and SignHealth, published in 2025, found 7% of respondents who required a professional to help with communication at appointments always had one.
NHS Humber and North Yorkshire Integrated Care Board (ICB) said the small number of qualified BSL interpreters was a long-term challenge needing national attention.
Millie said not having an interpreter made her “feel like I’m being ignored” and at risk of “missing out on essential information”.
According to Millie, staff have called her on the telephone to discuss appointments despite her explaining she cannot hear.
“They still carry on ringing, which is frustrating as I have to rely on other people to find out what they want – meaning I have no independence,” she added.
On the day of her surgery, she was told the interpreter had cancelled, but an available nurse was capable of basic signing.
Millie’s mother Joanne Neadley, who is also deaf, said: “It had been delayed, delayed, delayed and she just wanted it over with, because she couldn’t breathe.
“So to arrive at 7am and be told, ‘no interpreter’ it’s just not appropriate.”
Joanne said the nurse was “lovely”, but the situation was “not acceptable”. She added: “We want a proper BSL-qualified interpreter.”
According to RNID and SignHealth, more than 15 million adults in England are deaf or have hearing loss, with about one million unable to hear most conversational speech. There are an estimated 73,000 deaf BSL users.
The charities surveyed 1,114 people who were deaf or had hearing loss and lived in England.
Of the 208 respondents who said they needed a communication support professional, such as a BSL interpreter, 63% said one was rarely or never provided for appointments, while 28% said one was sometimes provided.
Their report, titled Still Ignored: The Fight for Accessible Healthcare, concluded that the NHS lacked “the systems in place to fulfil the right to accessible healthcare” within the deaf community.
It also found deaf people felt “disrespected”, “excluded” and often had to rely on friends and family members to translate.
Rachel Duke, 38, from Hull, said she was a sixth-generation member of a profoundly deaf family.
She described how the simple act of calling her GP surgery by telephone at 8am for an appointment was not possible and she had to ask someone to help.
She often arrived at appointments to find no interpreter had been arranged, which left her relying on family members.
On one occasion, she took her son, who is also deaf, to the GP and watched a display screen to see when his appointment was called.
“I was waiting a long time,” she said. “I went to reception and said, ‘I’ve been waiting for my son’s appointment’. They said, ‘We called your name, but you never came?’.
“There was nothing on the display screen.
“Then they said: ‘Sorry, we have to delay it now and book another appointment because you’ve missed it’.”
Rachel added: “I don’t want to rely on hearing people. I want to do it myself. Equality, that’s what we need.
“I feel like we’re at the bottom. We’re never understood.”
Heather Peachey, a level 6 BSL interpreter from Barton-upon-Humber, said she was the only qualified, registered interpreter in North or North-East Lincolnshire.
She began signing when her younger sister was diagnosed profoundly deaf aged five.
However, she said becoming a qualified interpreter was not easy.
“I had to stop part way because I ran out of money. I eventually became registered about 14 years ago after my dad left me the money to complete the training.
“It’s the same as learning any other language, it’s all self funded. There are very few universities offering BSL units.
“If you take somebody who’s never signed before, they’re probably looking at six, seven years to become competent and qualified as an interpreter.”
Signature, the BSL exam board, said learning to become a level 6 interpreter was likely to cost about £6,000, depending on the training provider.
‘Few and far between’
Only experienced, level 6 interpreters can attend medical appointments and surgeries, according to the NRCPD, external, a voluntary regulator for language service professionals.
It lists five interpreters living within 25 miles of Hull.
Sarah Regan, the residential manager at the Hull Deaf Centre, said qualified individuals were “few and far between”.
“There’s just not enough training. If you went into any school in Hull and asked them what they want to do, I doubt you’d get one coming back saying they want to be a BSL interpreter.
“The people who are learning sign language, paying out of their own pockets, should be applauded and encouraged financially with some money from the government.”
A spokesperson for RNID said equal access to healthcare was “a basic human right”, but their research had “exposed widespread failings affecting people who are deaf when accessing NHS services”.
The BBC asked NHS England and the Department of Health and Social Care to comment. Both referred us to the ICB, which works to reduce health inequalities across the Humber and North Yorkshire region.
A spokesperson for the ICB acknowledged interpreter provision needed to be improved and the body had been working closely with the Hull Deaf Centre to highlight the barriers people faced.
It had created new training tools for NHS staff, including films made with deaf people.
“The small number of fully qualified BSL interpreters in the region, and the seven‑year training route, is a long-term challenge that needs national attention,” the spokesperson said.
“We are working with NHS partners to make real and urgent improvements.
“This includes looking at the deaf patient journey from first contact through to complaints, making better use of BSL‑enabled technology, improving how interpreters are booked, increasing deaf awareness training for staff and making sure services meet the Accessible Information Standard.”
Khudee- Pakistan’s First Cafe Run By The Differently Abled
Our editor recently visited this restaurant, where she had a lovely lunch served by staff who need a little extra support in the workplace. She was very pleased to find such an organisation in Pakistan and asks local readers to support it as much as possible.
Cafe Khudee is another dynamic element by the Karachi Vocational Training Center for the empowerment of differently-abled individuals. Khudee is a state-of-the-art cafe and bakery with a stunning ambiance and exquisite taste. All menu is prepared by our specially-abled individuals under expert supervision. Khudee is a bright example of how far differently-abled individuals can go if they are treated and guided rightly. This cafe is a clear illustration of dedication and consistent work toward empowerment.
Wheelchair Camera ‘Is Milestone For Disabled Film-Makers’
A London film-maker with brittle bone disease has patented what he believes to be the world’s first wheelchair camera system.
Chris Lynch, from Stratford, east London, worked with engineers to make filming more accessible. The specialist equipment attaches a Steadicam to the side of a wheelchair with a mount, with the operator using a control panel placed on their lap.
Lynch’s system has already been used in productions like Channel 4’s Paralympic Homecoming and BBC documentary, In the Driving Seat.
The 44-year-old said: “This is a milestone within the disabled community. It means that I can shoot and be a camera operator, something I’ve wanted to do for a long time.”
Since 2007, Lynch has created a number of media companies specialising in documentaries and podcasts, but filming was always a problem.
“Filming wasn’t accessible, so I decided to create a camera system that could be not only be viewed as a gateway to disabled filmmakers, but a product that would add production value to any set,” Lynch said.
“I set up Diverse Made Media with a production arm because I wanted to make more of these wheelchair operated cameras and show aspiring disabled film-makers that production is possible for them.”
He worked with Jack Charge from Tilta, a company that specialises in cinematography equipment, and together they created the specialist kit.
Charge said: “This is a brand new system and is the first of its kind being mounted on to a wheelchair, which takes all the weight.
“It means that you have a wide variety of situations you can use this in like live broadcasts, music videos or even fast tracking shots for long periods.”
Lynch is now showcasing the system to studios, film-makers and students.
Jasmine Larkman is a university student at Liverpool Media Academy in east London and has hemiplegia.
She had her first go on the kit while at an arts conference last week.
Larkman said: “I can’t use my body on the right side, so with this kit there are so many ways you can use it. It’s really accessible for lots of people.”
Owen Tooth, director for Eastenders, is the long-running soap’s first wheelchair user to trial the system.
He said: “I’m most excited as a director, it opens up storytelling possibilities that were out of reach before.
“Looking at a system like this, there’s so much I can do, it feels so freeing.”
Lynch told the BBC that people within the disabled community had “resigned themselves to the fact that they can’t do these tasks” and it has always been a barrier for them.
He added: “That has been embedded for many, many years.
“I’d love to see more and more people be able to access this equipment across the industry. It’s exciting and I can’t wait to see where it takes us.”
lazy Saturday vibes as you can
Barbie® Introduces The First Autistic Barbie Doll, Championing Representation For Children Through Play

Mattel, Inc. unveiled today its first-ever autistic Barbie doll created with guidance from the autistic community to represent common ways autistic people may experience, process, and communicate about the world around them. This doll invites more children to see themselves represented in Barbie.
Developed for more than 18 months in partnership with ASAN, a non-profit disability rights organization run by and for autistic people that advocates for the rights of the autistic community, this doll joins the Barbie Fashionistas collection, which features the most diverse range of skin tones, hair textures, body types, and various medical conditions and disabilities.
“Barbie has always strived to reflect the world kids see and the possibilities they imagine, and we’re proud to introduce our first autistic Barbie as part of that ongoing work,” said Jamie Cygielman, Global Head of Dolls, Mattel. “The doll, designed with guidance from the Autistic Self Advocacy Network, helps to expand what inclusion looks like in the toy aisle and beyond because every child deserves to see themselves in Barbie.”
In close collaboration with ASAN, the Barbie design team made intentional design choices for the autistic Barbie doll to authentically reflect some experiences individuals on the autism spectrum may relate to. The autistic Barbie doll features and accessories include:
- Body: The autistic Barbie doll features elbow and wrist articulation, enabling stimming, hand flapping, and other hand gestures that some members of the autistic community use to process sensory information or express excitement.
- Eye Gaze: The doll is designed with an eye gaze shifted slightly to the side, which reflects how some members of the autistic community may avoid direct eye contact.
- Accessories: Each doll comes with a pink finger clip fidget spinner, noise-cancelling headphones and a tablet.
- Fidget Spinner: The doll holds a pink finger clip fidget spinner that actually spins, offering a sensory outlet that can help reduce stress and improve focus.
- Headphones: Pink noise-cancelling headphones rest on top of the doll’s head as a helpful and fashionable accessory that reduces sensory overload by blocking out background noise.
- Tablet: A pink tablet showing symbol-based Augmentative and Alternative Communication apps (AAC) on its screen serves as a tool to help with everyday communication.
- Sensory-Sensitive Fashions: The doll wears a loose-fitting, purple pinstripe A-line dress with short sleeves and a flowy skirt that provides less fabric-to-skin contact. Purple shoes complete the outfit, with flat soles to promote stability and ease of movement.
“As proud members of the autistic community, our ASAN team was thrilled to help create the first-ever autistic Barbie doll. It is so important for young autistic people to see authentic, joyful representations of themselves, and that’s exactly what this doll is. Partnering with Barbie allowed us to share insights and guidance throughout the design process to ensure the doll fully represents and celebrates the autistic community, including the tools that help us be independent. We’re honored to see this milestone come to life, and we will keep pushing for more representation like this that supports our community in dreaming big and living proud.” – Colin Killick, Executive Director, Autistic Self Advocacy Network (ASAN)
As part of the doll launch, Barbie is teaming up with advocates for the autistic community, including mother-daughter duo Precious and Mikko Mirage, autism advocate and creative entrepreneur Madison Marilla, and autistic fashion designer and visual artist Aarushi Pratap, to celebrate their lived experiences and lifestyles. The Barbie team filmed a unique video with them to capture and honor their personal experience with autism and delighted reactions to seeing the autistic Barbie doll for the first time. The video is available to view on the Mattel YouTube channel.
“Dolls have always brought me comfort, stability, and joy. I’ve been collecting Barbie dolls since I was four years old, and now this autistic Barbie will be one of my favorites,” said Madison Marilla, Autism Advocate and Creative Entrepreneur. “My good friend said these words to me, let yourself out and don’t hold yourself in, and it taught me how to educate people about autism. This autistic Barbie makes me feel truly seen and heard. I hope all the kids I’ve mentored feel the same when they see her, and I hope people who aren’t autistic feel educated and gain a better understanding of autism when they see this doll.”
Consistent with the Fashionistas dolls representing individuals with type 1 diabetes, Down syndrome and blindness, the autistic Barbie doll was named and created with the community’s guidance to allow more children to see themselves in Barbie. This doll, along with the entire Fashionistas collection boasts over 175+ looks, can help children better understand the world around them by encouraging doll play outside of a child’s own lived experience. It’s yet another step in making the Barbie brand a more inclusive reflection of the children who play with it.
Building on the importance of feeling understood and connected through play, beginning in 2020, Barbie set out to research the short- and long-term benefits of doll play through a multi-year study with researchers at Cardiff University, finding that playing with dolls activates parts of children’s brains involved in empathy and social processing skills. In recent years, the study has continued to build on these findings, suggesting that doll play could help develop social skills for all children, including those who display neurodivergent traits commonly associated with autism.
To celebrate the launch, Barbie will donate more than 1,000 autistic Barbie dolls to leading pediatric hospitals that provide specialized services for children on the autism spectrum, including Children’s National Hospital in Washington, D.C., Children’s Hospital Los Angeles (CHLA), and Rady Children’s Hospital Orange County. This donation is intended to bring moments of joy, comfort, and representation to the community, reinforcing the power of play to foster connection and confidence.
The autistic Barbie doll is now available on Mattel Shop and from major retailers.
Revolutionary Eye Injection Saved My Sight, Says First-Ever Patient
Doctors say they have achieved the previously impossible – restoring sight and preventing blindness in people with a rare but dangerous eye conditon called hypotony.
Moorfields hospital in London is the world’s first dedicated clinic for the disorder and seven out of eight patients given the pioneering treatment have responded to the therapy, a pilot study shows.
One of them – the first-ever – is Nicki Guy, 47, who is sharing her story exclusively with the BBC.
She says the results are incredible: “It’s life-changing. It’s given me everything back. I can see my child grow up.
“I’ve gone from counting fingers and everything being really blurry to being able to see.”
Currently, she can see and read most lines of letters on an eye test chart.
She is one line away from what is legally required for driving – a massive change from being partially sighted, using a magnifying glass for anything close up and having to navigate around the house and outside largely using memory.
“If my vision stays like this for the rest of my life it would be absolutely brilliant.
“I may not ever be able to drive again but I’ll take that!” she says.
With hypotony, pressure within the eyeball becomes dangerously low, leading it to cave in on itself.
It can happen if there is poor production of the natural jelly-like fluid inside the eye, following trauma or inflammation, for example.
Sometimes it’s a side effect of eye surgery or certain medications. Without treatment people can go blind.
Before now, doctors have tried using steroids and silicone oil to plump up the eye. But this can be toxic over long periods and doesn’t restore much vision.
Even when the cells at the back of the eye used for sight are working, the silicone oil is difficult to see through, causing blurry vision.
The experts from Moorfields decided to try a different approach with something they already had in their cupboard – a low-cost, transparent, water-based gel called hydroxypropyl methylcellulose or HPMC.
It’s already used in some types of eye surgery.
But rather than using it as a one-off, the Moorfield’s team decided to inject it into the main part of the eye as a new type of therapy.
When Nicki first had eyesight problems back in 2017, just after her son was born, she was initially given lots of silicone oil in her right eye, which was failing.
She says it had lost its normal shape and “sort of collapsed” or “crumpled like a paper bag” due to hypotony. The treatment did little to help.
And a few years later, her left eye started to fail in the same way.
“After I lost vision in my left eye, I thought, ‘there has to be something else we can try’,” she explains.
“Sheer determination. I was just like ‘I’m not giving up'”.
Her eye doctor Mr Harry Petrushkin said, together, they decided to do something entirely new – fill the eye with something that you can see through.
“The idea that we might be causing harm to somebody who has only really one eye with a treatment that may or may not work was nerve-wracking,” he recalls.
“We came up with this as a solution and amazingly it worked.
“Really, we could not have dreamt of her having the outcome that she has had.
“Somebody, who by all rights should have lost her vision in both eyes… is now living normally. That’s completely remarkable. We couldn’t have hoped for better.”
He says the same treatment could potentially help hundreds or even thousands of people each year in the UK. It comes down to whether they still have viable cells at the back of the eye that allow vision.
“We knew with Nicki there was vision to gain and she would get better if we could make her eye round and hard again.”
They’ve treated 35 patients so far, thanks to funding from the Moorfields Eye Charity, and have now published the outcomes of the first eight in the British Journal of Ophthalmology.
The treatment is given once every three to four weeks for around 10 months in total.
The researchers hope that with time, they will get even better at working out who could benefit.
“It’s been a fantastic story. The results are really promising but it’s early days,” says Petrushkin.
‘I’m Just A Disabled Kid But I Could Change The Law’
A 17-year-old boy with cerebral palsy said it was a “surreal moment” to have his petition on fire safety debated in Parliament.
Lucas has been campaigning for evacuation chairs to be compulsory in schools after being left “petrified” on his own in his wheelchair in an upstairs room when a fire broke out.
His experience at Hyde High School in November inspired him to launch his #NoStudentLeftBehind campaign to improve fire safety for disabled students.
“I’m just a disabled kid from Manchester and I am possibly changing the legislation. It’s amazing,” said Lucas, from Tameside in Greater Manchester.
“I want to see no student being left behind. They should feel safe.”
The small electrical fire at his school was quickly extinguished and no-one was hurt but Lucas said he was scared as he did not know the extent of the fire after being told to stay upstairs.
“I was petrified because I know how quickly the fire can spread,” he said.
“We all know the biggest killer in the fire is the smoke.”
More than 100,000 people have signed his petition for every school and college to have an evacuation chair and training.
His petition has since been debated by Parliament.
“It was just a surreal moment hearing all the MPs to say my name,” he said.
“They’ve done their research about me.”
‘Unbelievable’
Jacob Collier MP, who sits on the Petitions Committee, said it was positive that the Minister [for Schools Standards Catherine McKinnell MP] committed to meeting with Lucas.
“He’s done really well to get that commitment from the Minister and I think it’s great that the government is open also to acting on this so that we can ensure that disabled children are safe in school.”
Lucas has joined forces with the Emergency Group, a company that who provide life-saving emergency equipment including evacuation chairs and defibrillators.
Nick Cox, from the group, said: “I think it’s inspiring. It’s a story that needs to be told.
“For a 16-year-old boy when he initially started it, to get where we are now, it’s unbelievable.
“We have had literally, and I’m not exaggerating, hundreds of people saying to us that they’ve been in the same situation in schools, colleges, universities.
“It’s quite a common occurrence and it shouldn’t be, it really shouldn’t be.”
From The Tennis Court To The Pages Of Vogue
A woman with a rare genetic condition who has modelled for Vogue says she never wants to give up coaching tennis.
Alice Dyer, 20, from Arnold in Nottinghamshire, lives with connective tissue disorder hypermobile Ehlers-Danlos Syndrome, which causes her joint pain and extreme fatigue.
She discovered tennis when she was 14 years old after a “have a go” session at Nottingham Tennis Centre.
Now she uses her wheelchair to coach children between three and 10 years of age and says: “Kids don’t expect to have a disabled coach and they might not have met a wheelchair user before, so I am very grateful that I can introduce kids to that.”
Growing up, she recalls how she wore ankle and knee braces and wrist supports to prevent her joints from dislocating. At school she could not take part in activities like physical education (PE).
“It was hard to explain to my friends why I couldn’t do certain things,” she says.
Discovering wheelchair tennis gave her a “feeling of freedom”.
“I turned up and had a go,” she says. “I was rubbish, but I enjoyed it.
“It connects me to so many different people. It’s something that my body can do.
“I never thought it would lead to me working here as a coach.”
She was about 18 years old when she landed her first modelling job.
“By putting myself out there, it means that other people have someone who is like them in media,” she says.
Alice has worked with brands like Wimbledon e-commerce and online retailer Zalando. Her latest job was with Vogue Philippines in a portfolio celebrating diversity and inclusivity.
She found out she was in Vogue at home after her dad screamed her name on a Monday morning.
“It’s a surreal feeling and I haven’t fully processed it yet,” she says.
Alice had been approached for an editorial shoot in London in May last year, but after months of silence, she had no idea where the photos would end up.
“Not everybody gets into Vogue,” she adds.
Alice says the modelling industry is making moves with representation, but there is a long way to go.
“It’s one thing to have a disabled model in a campaign, but if the clothes don’t fit or aren’t accessible, that’s very different,” she says.
I Would Have Been Selfish Not To Share Twins’ Muscle Disease Diagnosis, Jesy Nelson Says
Singer Jesy Nelson has pledged to “shout from the rooftops” to campaign for all babies to get tested for a rare muscle disease at birth.
The former Little Mix star recently discovered her seven-month-old daughters have Spinal Muscular Atrophy (SMA) and will “probably never walk”, but the condition isn’t included in screening for newborn babies.
“That’s what’s frustrating,” she told ITV’s This Morning on Wednesday. “If this was the card I was always going to get dealt and there was nothing I could do about it, then it’s almost easier for me to accept.
“But when you know that there is something that can be done about it, and it is life changing to your child, that’s the part that I cannot accept.”
The singer became emotional as she told presenters Cat Deeley and Ben Shephard her life had “completely changed” since the diagnosis.
Nelson, 34, has called for SMA to be part of an NHS blood test that is normally carried out at five days old, and currently tests for 10 other conditions.
Speaking days after she posted a video on social media announcing her twins’ condition, Nelson said: “I have this platform, and I almost feel like I’ve got a duty of care to raise awareness about it.
“And a little part of me feels, and I don’t know if this is even crazy to say this, I feel selfish to keep this to myself and not potentially save a child’s life.”
Nelson added she has had to rapidly learn how to look after her daughters Ocean Jade and Story Monroe Nelson-Foster.
“It’s just so much to deal with whilst you’re also trying to deal with this horrendous thing that’s just happened.”
The singer said doing that while also simply trying to be their mum was “the part that I’m still struggling with”, and was comforted by Deeley as she became emotional.
“I won’t lie. The part that really gets me, is I just want to be their mum, I don’t want to be a nurse.
“So it’s hard, but, yeah, I just want to reiterate that if this is caught [diagnosed] from birth, it’s just life changing.”
‘They are still smiling’
She added that it “makes me so sad” to watch back videos of her girls and now be able to spot the signs that their legs were gradually moving less during their first weeks.
“That’s how quick it is. And that is why it is so important and vital to get treatment from birth, and it is detected from birth,” she said.
The girls have now had treatment in the form of a one-off infusion, she explained.
“It essentially puts the gene back in their body that they don’t have. It stops any of the muscles that are still working from dying.
“But any that have gone, you can’t regain them. That’s why if you catch it early [it’s better]. Now it will just be down to a case of constant physio.”
She continued: “We’ve been told that they will probably never walk. They’ll probably never regain their neck strength. They are going to be in wheelchairs.
“But there have been so many stories where parents have been told this, and their children have gone on to do incredible things. So I believe that you’ve just got to manifest this into existence.
“They are still smiling. They’re still happy. They have each other, and that’s the main thing that I’m like so grateful for, because they could be doing this by themselves, but they’re twins and they’re going through this together, and I think it’s beautiful.
“So all I can do is just try my best to be there for them, give them positive energy, keep doing physio.”
On Tuesday, Health Secretary Wes Streeting told ITV News that Nelson was “right to challenge and criticise how long it takes to get a diagnosis”.
He said he was “determined to look not just at screening for SMA, but to make much better use of genomic medicine”.
In 2021, a life-changing gene therapy drug called Zolgensma was approved by the NHS to treat babies with the disease.
According to the charity SMA UK, the drug delivers a healthy copy of the affected gene to the body, but timing is critical because irreversible damage may have already occurred in the nervous system.
Scotland will start routinely screening babies for SMA from the spring, and the National Screening Committee is currently reviewing whether to introduce it across the UK.
Nelson added her voice to a campiagn by SMA UK to introduce routine screening to the NHS newborn blood spot test, which currently looks for conditions including cystic fibrosis, sickle cell disease and a range of inherited metabolic diseases, but not SMA.
An NHS spokesperson said three new treatments for SMA had been rolled out since 2019, helping hundreds of children.
“The UK National Screening Committee is looking at whether the NHS should introduce routine screening to identify the condition in early life via a heel prick blood test – and the NHS is supporting further evaluation to inform the Committee’s decision.
“The Generation Study is also evaluating whether genomic sequencing could be adopted more widely as part of standard newborn screening in the NHS, including testing for SMA.”
‘I’ve Been Denied Cervical Screening Four Times’
A woman who uses a wheelchair said she had “given up” trying to have a cervical screening after turning up for an appointment to find she could not get inside a treatment room.
Emily Salter, who is unable to walk after falling from a 9m (30ft) cliff seven years ago, said she had tried to arrange for the screening, known as a smear test, four times but appointments had been cancelled due to accessibility issues.
The 33-year-old, from Preston, Lancashire, said: “I thought the NHS would be a safe place for me to go without having to worry or panic beforehand.”
An NHS England spokesperson said screening services are “expected to make reasonable adjustments” to support women with disabilities.
This includes “ensuring suitable facilities and access to specialist equipment where needed”, the NHS spokesperson added.
A survey by the Spinal Injuries Association found two-thirds of women with physical disabilities had not been able to attend a smear test appointment.
Just under half of those cited accessibility issues as the top reason for this.
“When I’m on the phone I always say I’m in a wheelchair, I can’t stand up, just to make them aware” said Salter.
“You turn up and the building has steps to go inside. The next one, the room was that small that the wheelchair wouldn’t fit next to the bed.
“And then the fourth one, they actually rang me to cancel because they said it wasn’t accessible.”
‘Entirely preventable’
Dharshana Sridhar, campaigns manager at the Spinal Injuries Association, said: “The system is not made for women’s health to start with and then it’s even worse for women with disabilities.
“And then some of the barriers are actually entirely preventable, like inadequate equipment, like a lack of height adjustable examination beds, but none of this has been happening for decades.”
Local screening teams can “offer practical support such as longer appointments at accessible sites and alternative clinic options” to help women with physical disabilities, the NHS spokesperson said.
But Salter said she had “given up”, adding: “I don’t know what more I can do to access these services.”
“I just think it’s very sad that we’re put in a position where we feel bad about ourselves because we can’t access the healthcare,” she said.
“I’m grateful for what the NHS has done for me. They’ve showed me I can live again.
“Life doesn’t end when you have a spinal cord injury but I want my life to continue and if I can’t have these checks for cancer then they’re not going to be able to catch it quick enough.”
Sally Jones, from Ellesmere Port, Cheshire, was left paralysed from the waist down after a motorbike crash in January 2020.
The 45-year-old has a history of abnormal cells in the family so she said she had been left feeling worried that she had not been able to have the test.
“I try to put it at the back of my mind,” she said.
“I think given the family history as well, I’m probably one of the people that should be going for regular tests.
Sally said she had also been left humiliated after she was given no option but to have her coronavirus vaccination outside due to a lack of access at the site.
“It’s a battle,” she said.
You’ve got to be proactive and you’ve got to row your own boat and you’ve got to keep on nagging to be heard.”
‘My Student Inspired Me To Spread Braille Message’
The founder of a braille and large print business said she hoped to make the Isle of Man a more “accessible and inclusive” place for people with visual impairments.
Natasha Molyneux-Smith spent years working at a secondary school with Evie Roberts, a 16-year-old Manx girl who is completely blind.
“Just because we only have a handful of braille users does not mean that we restrict their access to text,” explained Natasha.
Having started her company Dot and Type in September, Natasha has called on public venues and workplaces to offer more resources for visually impaired people.
She said thousands of people also travelled to the island for the TT Races, and the island had an opportunity to be a “flagship for accessibility if all of our menus were (also made available in) braille and large print”.
Evie, who was born with bilateral anophthalmia, said working with Natasha had resulted in the “first time I’ve ever seen a menu”, something she described as “an amazing experience”.
The teenager said it gave her added independence as well as taking away the responsibility from someone else to read the entire menu to her.
She explained: “For someone with sight when you go out for a meal, you just go into a restaurant and look at what you want to eat and you don’t think about it.
“I’ve never had that.”
Natasha said: “That really struck home to me. It made me realise this is why I’m doing my business.”
One of the first companies on the Isle of Man to introduce braille and large print menus is Just Pizza and Pasta in Douglas.
Owner Mitch Sorbie said he wanted to make sure no-one felt excluded.
He said he sometimes hosted groups from local charity Sight Matters.
“I’m looking forward to the first time they come in and we give them the menus… to see their facial expression of being included, I think that’ll be great,” he said.
It was the restaurant’s way of showing “someone else is thinking about them”, he added.
Payout Over Sign Language Failure For Man In Care
A council in west London has apologised after failing to provide adequate support for a deaf man receiving care who required British Sign Language (BSL) interpreters.
Hammersmith and Fulham also agreed to pay the man’s granddaughter £450 and “review its processes” on interpreters with BSL.
The Local Government Ombudsman found several faults with the service provided by the council, including that staff at a care home, referred to as Care Home B, were not trained in BSL, contrary to the man’s care requirements.
A council spokesperson said they “wholeheartedly” apologise to the family and that they are working to ensure the same issues do not arise again.
The ombudsman said the man, referred to as Mr Y, had a number of health conditions, was profoundly deaf and used sign language to communicate, according to the Local Democracy Reporting Service.
His daughter, Ms Z, was his main carer. Miss X, his granddaughter, is a qualified BSL interpreter.
In March 2024, Mr Y was discharged from hospital following which he received a care plan.
It noted that his first language was BSL and that he required a BSL interpreter although, because of difficulties finding carers with such skills, Ms Z was asked to help them communicate with Mr Y.
Council ‘to review processes’
In September 2024, Care Home B told the council it had met with Mr Y’s family and that they were happy for him to move there as long as the BSL outreach support was provided.
The care plan said care home staff should learn basic BSL skills, but the home said it had received no training in BSL or deaf awareness.
In December 2024, Mr Y was transferred back to another care home shortly after which he was admitted to hospital, where he died.
During this period Miss X had complained to the council on various points regarding her grandfather’s care.
A series of actions were agreed with the council, including apologising to Miss X, making a payment to her of £450 and reviewing its processes regarding the provision of BSL interpreters.
A Hammersmith and Fulham Council spokesperson said: “We wholeheartedly apologise to the family. Finding specialist British Sign Language and deaf relay interpreters for care homes can be very difficult and we’re working to make sure this doesn’t happen again.”
Ex-EastEnders Star’s Ultra-Swim Of Length Of Lake Geneva
A former EastEnders actor from Brighton is planning to take on an epic ultra-swim of the length of Lake Geneva to raise money for his son’s school.
Will Ellis, who played villain Theo Hawthorne, is planning the 70km (43 miles) swim in August. It has only been completed by 16 people so far.
His son Odie has Mowatt-Wilson Syndrome, affecting his development, and the swim will raise money for his school, Downs View, in Woodingdean, Brighton.
“They’re in desperate need of funds to keep the school running so I thought it was a great opportunity to do something really crazy and raise some money,” Ellis said.
As well as being famous for playing Theo in the soap in 2023, Ellis is also well-known as an ultra-endurance swimmer and has a podcast on open-water swimming.
He has swum the English Channel and around Jersey, which he says he will do again as part of his training for Lake Geneva.
His six-year-old son is non-verbal and doctors said he may never talk or walk, although he is now walking with the help of splints.
Ellis said: “Life expectancy can range because no-one really knows, so we have to be grateful for every day with him, grateful that he’s happy.”
Downs View is hoping to raise £15,000 for a new soft play, as the school’s room needs refurbishment and cannot be used in its current condition.
Head teacher Vanessa Hickey said: “Lots of our children here have complex needs, a lot of them have autism, communication issues, and a learning disability as well.
“What’s important are the skills the soft play develops, like dexterity and motor skills, as well as it being an outlet for energy, particularly on wet days.”
Ellis says he expects to be in the water for between 24 and 30 hours, without a wetsuit, and despite a busy training schedule, there are no guarantees he will complete the challenge.
“You have to just turn up for these swims, controlling what you control, because there is a lot of luck. and it has to shine on you that day.”
Selfie at the wacky wheels Christmas party 2025
a video that I created using black white photos of my chosen nieces as I’m proud to be an auntie by choice
when the evening in the life with me diamond art Christmas decoration making edition please take a moment to watch my evening in life by clicking on the video
Video of the stage dancers at the 2025 panto
video of the finale of the panto that I enjoy the most since I’ve been going for many years now with different social groups and friends for
a video of me at Friday club’s Christmas party 2025
‘Lack Of Physio Leaving Our Children To Suffer’
Lack of physiotherapy is putting the health of children with physical difficulties at risk, a group of parents has said.
The families of children with scoliosis – curvature of the spine – say Sirona Care and Health is failing to supply experienced physiotherapists to Claremont School in Bristol.
The complaints follow a decision by Sirona to reduce the number of physiotherapists at the school and instead instruct unqualified teaching staff how to manage scoliosis.
After being contacted by the BBC, Sirona commissioned a review of its children’s therapy service. A spokesperson said its priority was “the safety and wellbeing of the children and families we support”.
One of the parents, Helen, has a 15-year-old son named Sam who was born with severe cerebral palsy. As part of that condition, his spine is curved.
Helen said his scoliosis could be managed with appropriate physiotherapy and equipment at Claremont, a special school.
But the mother, from Bedminster in Bristol, claims community interest company Sirona made his scoliosis far worse from May 2024 to March 2025 as his school chair had been set up the wrong way round.
She said that his ribs looked stretched in X-rays by March 2025 and that his whole torso was becoming deformed.
“I just watched his back concertina,” she said. “Over a 10-month period, Sam’s spine went from 20 degrees to over 90 degrees and after a catastrophic collapse, he’s now in excruciating pain. It was entirely preventable.”
She added: “Sam is in excruciating pain because his scoliosis means the top of his pelvis is rubbing on his bottom rib.
“This in itself won’t necessarily shorten his life, but our choice, as parents, is to decide whether to leave him in agony for the rest of his life, or let him undergo a lengthy and risky operation which he may not survive.”
Sirona announced a reduction of physiotherapists at Claremont in June 2024, saying it would boost home visits.
Parents have told the BBC the decision led to experienced physiotherapists handing in their notice.
Helen wrote a complaint about the changes to Sirona but it described her letter as “aggressive and abusive”.
She said that, as a consequence, she withdrew her consent for Sirona to treat Sam.
Instead, she said she is using her life savings to pay for a private physiotherapist, costing £90 an hour.
Another parent, Julian, said he was also unfairly accused of being aggressive by Sirona.
He said a formal investigation had been carried out into his daughter Gemma’s care but he “didn’t see any action” so continued to contact the company.
Julian said he and his partner then received a letter saying Sirona had been informed they had been “aggressive and threatening” towards the therapy team.
Sirona told them they were being given a “second stage warning about modifying their daughter’s care”, Julian said.
The company also told the parents that their daughter would no longer be seen in their home and would be seen only at school, with a member of staff present in order to “protect the therapists”, the father said.
He added: “We were not being threatening. When we challenged them on [the warning] they could not give us a solid example of why that was done.”
Julian also said because the family had “stepped in” to make sure her physio treatment had continued, they had manage to avoid complication such as acute pain, bowel blockages, interrupted sleep and seizures which said could “all be life threatening”.
The group of parents, whose children all attend Claremont, have now written an open letter that criticises Sirona’s cuts to school physiotherapy.
The letter says a number of parents have contacted Sirona and the special education needs team at Bristol City Council to raise their concerns about the “profoundly negative impact on the development of our children at Claremont”.
‘Deeply concerned’
The letter continues: “The absence of therapists on a daily basis is not acceptable and is having a detrimental effect on them and represents a cut in service.”
The parents say all of their children have ECHPs – an education, care and health plan, which is a legal document outlining their needs, including therapy, and which unlocks funding.
“As their parents, we want to know what is happening with this funding,” the parents write.
“What is being done to reinstate the provision our children need?
“We are also deeply concerned about the poor communication regarding the changes, which has come third hand without any explanation.”
‘We will act’
Sirona declined to comment about the families’ allegations but told the BBC its external review, which began on 1 December, is expected to run until mid-February.
In a statement, spokesperson Mary Lewis, Sirona’s chief nursing officer, said: “We have ensured that all concerns raised with us have been formally recorded and will be shared with the review team, and we are working closely with our partners throughout the process.
“The inquiry will look in depth at how the service is operating across all settings. It will identify what is working well, what may need to improve, and whether any factors within Sirona or the wider system could impact the delivery of the standard of care we expect.
“An Appreciative Inquiry is a structured, transparent and strengths-based method that examines the experience of those receiving care and those providing it.
“We will act on the findings of the review. Our priority remains the safety and wellbeing of the children and families we support, and ensuring our staff have the conditions they need to deliver high-quality care.”
the very musical performance of Aladdin that I saw in panto this year 2025 watch the video to see some of what I saw in this video blog
‘High-Tech Prosthetic Arm Would Be Life-Changing’
A teenager born without the lower part of her right arm is seeking to raise £20,000 to buy a high-tech bionic arm she said could transform her life.
Sadie, 17, from Winnersh, previously used a prosthetic arm as a young child but stopped as she felt it was hampering her independence.
But now, with her potentially starting university next year, she said the Hero Pro would enable her to complete everyday tasks that she can sometimes struggle with.
A campaign has currently raised £4,500 with other fundraising set to take place in early 2026, including a runner who is set to take on the Thames Path Ultra Challenge for Sadie’s benefit.
“Coming up to 18, I need more independence and I have always relied on my parents a bit. It really hit me when I went to secondary school and realised I was doing a lot more by myself. Two hands would make life a lot easier,” Sadie said.
She recalled that her earlier use of the prosthetic arm “felt like a nuisance”.
But she said the Hero Arm, which can pick up a maximum of 25kg, would be life-changing.
Sadie said tasks that other people might take for granted, like tying her hair and cooking, can be difficult.
“It sounds silly but they’re the little things, everyday tasks that Sadie wants to do alone now. She doesn’t want me and her dad helping her,” Sadie’s mum Sarah added.
“I feel so emotional but in such a fantastic way,” she added.
“It’s great to see. Sadie is a really determined character and always has been from the day she pulled off her prosthetic arm and threw it down.”
visiting the Christmas selfie decorations in my local town 2025
Sensory Grotto Makes Santa Visits Accessible
A charity has built a sensory grotto to make visiting Santa accessible to all.
Focus Birmingham, which cares for people with visual impairments and complex needs, aims to create a sense of calm with the grotto’s adaptable soft lights, gentle sounds and different textures.
It created the experience to make Christmas more inclusive and ensure that there was a “safe space” for everybody to enjoy a visit with Santa.
“The family’s reactions are amazing to what we do, it fills my heart all year,” staff member Thomas Ward said, adding that it gave “something to the wider community”.
Mr Ward said that the charity celebrated all events across Birmingham and Christmas time incorporated “lots of love”.
“We do this to give an opportunity for everyone to see Father Christmas, regardless of their age, their additional needs,” he said.
CEO of Focus Birmingham Kate Burke said the grotto was just one of many accessible events that the charity held with others, including Christmas fetes, bingo and sing-alongs.
“It’s so important because we believe everybody has the right to live life to the full and reach their potential,” she said.
Ms Burke said that Christmas could be a time with more barriers for those with care and support needs, so the charity made sure people had the same opportunities.
The charity’s specialist mini buses cost more than £400,000 a year to help keep the centre accessible.
It appealed for support for its Christmas campaign this year to help fund the transport service.
Adam Pearson Is Worried About Some Uses Of AI
Dr Shani Dhanda speaks to us from Tokyo where she’s delivering a keynote speech at the world’s first Accountability Summit which has brought together 500 companies who made disability pledges in the past two years to see just how well they’re doing. Plus she reveals how she would ideally celebrate IDPD
CEO of Paralympics GB, Dave Clarke, tells us what he thinks about marking the day and reveals the latest research about the number of disabled people getting involved in sport and what’s holding others back.
Plus, we have Hollywood film star, presenter and campaigner, Adam Pearson, in the house. He’s just been announced as the patron of Face Equality International. He talks about the challenges AI can pose for someone with a facial difference and gives us the inside scoop on his next big film role….a man he once loathed as a child, but has come full circle to love.
Intrigued? – Get your party hat on and take a listen!
Santa’s Little Yelpers Socialise With Saint Nick
Guide dog puppies have been preparing for Christmas with a visit to Santa’s grotto as part of their early socialisation training.
A dozen puppies and their raisers, who care for them during the first year of their lives, explored the grounds and gardens at Delapré Abbey in Northampton before seeing Father Christmas.
It was organised by sight loss charity Guide Dogs to help build their confidence in unfamiliar environments.
Claire Purr, the charity’s puppy development adviser, said it served as a reminder of why the charity needed to triple the number of its volunteer puppy raisers in the UK.
“Santa’s been amazing, and it is a fun thing, but actually it’s really good for their training too for them to learn to be around all these different things,” she said.
“There would be no guide dogs without puppy raisers; we need people to raise our puppies to help them on their journey to be successful guide dogs.
“We don’t have that many homes at the moment, so it’s been a challenge this year getting people on board.”
Linda Whitwell, one of the county’s most experienced puppy raisers, said the festive visit was “something different” for her 12-week-old labrador called Hollie.
“She [Hollie] seemed to really enjoy it,” she said.
“It’s nice that it’s all different experiences and it’s good for them anything like that.”
There are 12 volunteer puppy raisers in Northamptonshire, who introduce them to different experiences and prepare them for their formal guide dog training.
If they complete their training, they go on to become assistance dogs for people with sight loss.
Ms Whitwell – looking after her 17th dog – said the role of a puppy raiser “is very rewarding”.
“Although the cat wouldn’t agree with me,” she joked.
“It’s a lot of fun, it’s all experiences, socialising them and going to different places.
“If we go on holiday, we take them with us because it’s all new scenes and the seaside.
“People often say to me ‘I’d love to do it, but I just couldn’t let them go’.
“You’ve got to get the mindset [that] it’s not my dog and I’m doing this to change somebody’s life.”
Disabled Adventurer Starts South Pole Challenge
An adventurer has begun an attempt to reach the South Pole and break a record for the longest-ever sit-ski expedition by a disabled person.
Darren Edwards, from Shrewsbury, who is paralysed from the chest down, hopes to cover 137 miles (222km) over a period of 20 days
He is raising funds for charity Wings for Life, which is researching cures for spinal cord injuries.
In an update from base camp before he set off, Mr Edwards said his sit-ski had been adapted to become more “Antarctic proof” with rebuilt foot plates and a sheepskin padding.
The current record for the longest sit-ski to the South Pole stands at almost 69 miles (111km).
Joining him on the South Pole expedition are explorer Lucy Shepherd, Chief Scout Dwayne Fields and filmmaker Matthew Biggar.
The team will camp overnight, navigating temperatures as low as -30C and the risk of extreme winds, altitude sickness and snowstorms.
Former mountaineer and army reservist Mr Edwards was paralysed in 2016 at the age of 26 after a rock climbing accident.
Since then, he has been part of the first disabled team to cross Europe’s largest ice cap, Vatnajokull in Iceland, and undertaken seven marathons in seven days on seven continents.
He has also led a rowing crew across the English Channel and kayaked from Land’s End to John O’Groats.
Artist Nnena Kalu Earns ‘Historic’ Turner Prize Win
Nnena Kalu has won this year’s Turner Prize, the UK’s most high-profile art award, for her “bold and compelling” sculptures and drawings – and has made history as the first artist with a learning disability to win.
The judges praised Kalu’s brightly coloured sculptures – which are haphazardly wrapped in layers of ribbon, string, card and shiny VHS tape – and her drawings of swirling, tornado-like shapes.
Kalu, 59, is an autistic, learning disabled artist with limited verbal communication.
Charlotte Hollinshead, who has worked with her for 25 years, said on stage at the ceremony: “This is a major, major moment for a lot of people. It’s seismic. It’s broken a very stubborn glass ceiling.”
‘Idol, legend, winner’
In a moving speech delivered alongside Kalu, she said: “This amazing lady has worked so hard for such a long time.
“It’s wonderful she’s finally getting the recognition she rightly, rightly deserves.”
Glasgow-born, London-based Kalu was announced as the winner of the award – and its £25,000 prize money – at a ceremony in Bradford, the UK’s current city of culture, on Tuesday.
She accepted the honour while wearing a rosette bearing her photo and the words: “Idol, legend, winner, whatever.”
Kalu has been gradually gaining recognition in the art world in recent years after working as a resident artist with Action Space, which supports artists with learning disabilities, since 1999.
‘Incredible amount of discrimination’
Ms Hollinshead, her studio manager and artistic facilitator, said: “We are so happy that Nnena’s talent and beautiful work is now out in the world for you all to see this complex artist who creates gorgeous, complex forms – all while listening to disco music, often as loud as possible.
“Nnena’s career reflects the long, often very frustrating journey we’ve been on together… to challenge people’s preconceptions about differently abled artists, but especially learning disabled artists, an important creative community so undervalued.
“When Nnena first began working with Action Space in 1999, the art world was not interested.
“Her work wasn’t respected, not seen, and certainly wasn’t regarded as cool.
“Nnena has faced an incredible amount of discrimination, which continues to this day, so hopefully this award smashes that prejudice away.
“Nnena Kalu, you’ve made history!”
‘Beautiful intricacy’
Kalu’s work has divided opinion among art critics, but the Turner Prize judges were impressed by the “really compelling sculptures and drawings that could only be made by Nnena”, according to the jury chairman, Tate Britain director Alex Farquharson.
Her drawings, which come in sets of two or three near-identical shapes, have “a beautiful intricacy to them” and “look like swirling vortexes”, he said.
Her sculptures, meanwhile, are hanging shapes covered in reams of re-purposed materials including fabric, rope, parcel tape, cling film and paper.
They resemble three-dimensional versions of abstract expressionist paintings, Mr Farquharson said.
“But they’re not paintings, they’re not flat on the wall. They’re suspended in the space that you’re in, like brightly coloured rocks or creatures.
“They’re at almost your eye level. Although there are no figurative features at all, they appear to be communing among themselves and with you.
“The use of materials is highly unusual, including video tape that gets wrapped round and round.
“The colours and the lines the materials make are very like brush marks translated into three dimensions. They’re very gestural, they’re very expressive, they’re very compelling.”
‘Quality and uniqueness’
The judges deliberated for two or three hours, Mr Farquharson said, and stressed that their choice of winner was based purely on merit.
“The result wasn’t about wanting, first and foremost, to give the prize to Nnena as a neurodiverse artist. That wasn’t a driving factor,” he said.
“It was an interest in, and a real belief in, the quality and uniqueness of her practice, which is inseparable from who she is.”
It is a historic moment, though, he told BBC News.
“It breaks down walls between, if you like, neurotypical and neurodiverse artists. It becomes really about the power and quality of the work itself, whatever the artist’s identity is.
“So maybe what’s historic about it is it’s one more move to include really great neurodiverse artists in the picture we present of art today.”
The result was announced at a ceremony at Bradford Grammar School, the former school of artist David Hockney.
Works by all four shortlisted artists are currently on show at the Turner Prize exhibition at the nearby Cartwright Hall gallery, which will run until 22 February 2026.
The other nominees were Rene Matić, Zadie Xa and Mohammed Sami, who will receive £10,000 each.
The Turner Prize has been the UK’s most coveted and controversial art award since it was founded in 1984. Past winners include Lubaina Himid, Jeremy Deller, Grayson Perry, Steve McQueen and Damien Hirst.
Blind Footballer Robin Williams Dies Aged 37
The news was shared by IBSA Blind Football:
It is with profound sadness that we share the news of the passing of Robin Williams. Robin passed away at his home on Monday evening after a lifelong battle with (retinoblastoma). He was just 37 years old.
Robin was a former England Blind Football International player who loved playing football for his country (in total he played 106 times and scored 30 goals, including London 2012 Paralylmpic Games).
The whole Blind Football community mourns the loss of a true legend. Our thoughts are with his loved ones during this difficult time.
When Madeline Alterman started Artbox in Islington in 2011, she only had £300, a handful of volunteers and an idea – to support artists with learning disabilities and autism.
Now her organisation works with more than 90 artists each week, providing studio space, materials and tuition.
Some of their works have been exhibited, commissioned and sold, with artist Shruti designing the advent calendar for beauty brand Lush, and Seatton painting the cover art for Irish music artist CMAT’s second studio album, Crazymad, for Me.
Meanwhile, Richard’s painting called SHIP was featured in last month’s edition of the House and Garden magazine.
Artbox was born out of Ms Alterman’s belief that adults with learning disabilities need “real opportunities” rather than “token gestures”.
“I was hearing the same issues again and again: loneliness, isolation, nothing fulfilling to do, not feeling valued, shrinking budgets and almost no access to paid or purposeful work,” she explained.
Ms Alterman, who has a background in art and psychology and co-directs the organisation, grew up with a younger brother who has learning disabilities.
“We were encouraged to include him in everything, to advocate for him, to understand the system, and to push for better support.”
‘Mummy, Daddy, I’ve sold a painting!’
I visited the studio on a Thursday afternoon for one of the week’s livelier sessions, with the Backstreet Boys blasting through the speakers.
“Everyone here presents with their own differences,” said tutor Katie Parsons.
“You can’t just say ‘people with autism hate loud noises’ – that’s not the case. Certain people with autism hate loud noises in the same way that certain people without autism hate loud noises.”
Seeta, 52, arrived with a picture of a parrot she had seen on TV and planned to draw. It took her approximately an hour and a half to create an expertly drawn and coloured rendering.
Diagnosed with meningitis at six months old, Seeta said she has epilepsy and panic attacks, and was in comas throughout her youth.
At the age of 20, she sold her first painting.
“I ran home shouting, ‘Mummy, Daddy, I’ve sold a painting!'”
Violet started attending the sessions at Artbox when her mother died.
“When I first joined, I only wanted black and red because I was grieving so much,” she said.
“Then I came out of the light and saw all the bright colours and suddenly it was like, ‘I can do this, I can be an artist now’.”
Violet is also volunteer and workshop leader for Artbox – the workshops help the organisation to raise funds and build confidence in the artists who lead them.
One artist with Down’s syndrome returned to the Francis Crick Institute, which had previously worked with her as a patient, to deliver a workshop for World Down’s Syndrome Day.
Ms Parsons, herself a practicing artist, said she was inspired by both the confidence and “amazing lack of preciousness” possessed by the artists.
“One of their most incredible qualities is that they don’t have that self-conscious nervousness about creating that a lot of us do – second-guessing whether we’re doing the right thing and whether we’re doing it correctly,” she said.
She added the organisation would keep finding ways for artists’ work to be “seen, celebrated, and taken seriously”.
“When adults with learning disabilities receive the right environment – properly staffed, well-resourced, and grounded in respect – they thrive.”
videos of singing happy birthday and bringing the cake out in Dinner Club and General celebrations for my birthday
Nigella Lawson Opens Training Pub For Young People
Food writer and TV chef Nigella Lawson has opened a pub designed to help prepare young people with learning disabilities or autism for employment.
The North Star, set up by Brighton-based charity Team Domenica, provides the young people with real-world training opportunities that allow them to build their skills, confidence, and independence.
Alongside Ms Lawson, the Brighton venue was opened by Baroness Rosa Monckton, who founded the charity in honour of her daughter, Domenica, who has Down’s syndrome.
Georgia Pink, the charity’s enrichment coordinator, said: “Our main goal is to empower… and help them gain paid employment.”
The charity was founded in 2016 after Domenica left college and faced a lack of opportunities typical for young adults with learning disabilities.
Just 4.8% of adults with a learning disability and autism are in employment in England, according to figures from the NHS.
Through the programme, Team Domenica has said that 86% of candidates progressing into employment have stayed in their position for more than two years.
Ms Pink, who has worked at the charity for almost six years, called all the candidates “incredible”.
She said they do everything “with real confidence and determination”.
“Their self-confidence and sense of belonging in the community,” Ms Pink added.
“Feeling appreciated by employers and colleagues is really important.
“Everyone should have the right to do that,” she continued.
Educate, Don’t Segregate: Free Online Rally For Inclusive Education
Join the Rally for Inclusive Education
Disabled People’s Organisations, activists, parliamentarians and supporters are uniting to oppose the government’s agenda that increases segregation in education. Together, we are demanding an education system that values Inclusive Education and the rights of all Disabled people.
We demand an end to:
- Building new special schools and SEN Units
- Delays to the School’s White Paper on SEND reform
- Funding structures that favour segregated schooling
- Cuts to SEND resources in mainstream schools
- The use of force, restraint, and seclusion in educational settings
- Systemic barriers that exclude Disabled people
- Government failure to uphold the UNCRPD commitment to Inclusive Education
Date: Wednesday, 10 December 2025
Time: 6:30pm – 7:30pm
Location: Zoom
Access BSL interpreter and caption provided
Speakers & Contributors
Co-Chairs:
- Rick Burgess – Greater Manchester Coalition of Disabled People
- Michelle Daley – ALLFIE
Confirmed Speakers:
- Marsha de Cordova MP – Battersea
- Svetlana Kotova – Inclusion London
- David Buxton – Action on Disability
- Sharon Smith – SEN Jungle
More speakers to be announced…
Defend the right to Inclusive Education for everyone.
Hosted by ALLFIE – The Alliance for Inclusive Education
PIP Withdrawn From Amputee Over Cricket Video
The family of a man who lost his leg when he was two years old have asked for a rethink of a decision to strip him of his disability benefits and force him to pay back £36,000.
Shaun Rigby from Telford had his Personal Independence Payment (PIP) withdrawn after a video emerged, showing him take part in a game of cricket.
But his family said: “Playing cricket does not negate Shaun’s disability; it showcases his determination to lead a fulfilling life despite it.”
The Department of Work and Pensions said its decision had been backed by an independent tribunal and PIPs were “awarded based on how a condition impacts a person’s day-to-day needs, as opposed to the condition itself”.
In an online petition, Mr Rigby’s family said he had “overcome incredible odds since losing his leg below the knee in a tragic tractor accident when he was just two years old”.
They said despite his physical challenges, the 37-year-old had tried to “live as fully as possible, embracing activities like cricket not only for his own mental and physical health but also to share joyful moments with his family”.
Mr Rigby said he used to play for England’s disability cricket team, before eventually having to give it up.
He said: “I stopped playing about 2014, just because I couldn’t do what I wanted to do, my body was sort of breaking down.”
Since then, he said the pain became worse and he was successful in applying for PIP in 2016 and a Motability car three years later.
But the DWP decided to withdraw both after their attention was drawn to the video of him playing cricket in 2023.
His family said it had been “a light-hearted community cricket match”.
They argued that “participating in adaptive sports is a well-known form of rehabilitation and psychological well-being for individuals with disabilities”.
The decision to strip him of his benefits took away his independence and his ability to care for his family, they said.
Mr Rigby said he understood why the DWP had made the decision, but wanted the government department to know he played despite his condition and did it partly to inspire others.
He said he would undergo six days of “torture” after playing, because of the pain.
The family has asked the DWP to reassess his case and reverse the decision.
His wife, Lauren, said losing the PIP payments was difficult in itself, but the thought of having to repay the £36,000 was causing the family “stress and worry”.
“Do they want us to go into poverty?” she asked.
Mrs Rigby added she wanted to push back at some of the negative comments they had received after it was announced he would lose the payment, but that there had been “nothing but good comments” since the online petition was launched.
The DWP said: “Following Mr Rigby’s appeal, where he was able to challenge his benefit entitlement, an independent tribunal agreed with DWP’s decision.”
It also said that every PIP claim was different, because of individual circumstances “including age and the ability to manage a condition without supervision or assistance”.
Mr Rigby is waiting to hear what the weekly repayments will be on the £36,000 and believes it could be up to £35 a week.
The DWP said it was committed to working with anyone struggling with repayment terms.
Streeting Orders Review Into Mental Health And ADHD Diagnoses
Health Secretary Wes Streeting is launching an independent review into rising demand for mental health, ADHD and autism services in England.
It will look at both whether there is evidence of over-diagnosis and what gaps in support exist.
The government said it was already investing in expanding services, but there are long waits for therapy in many areas.
NHS figures show rates of mental health problems and ADHD have increased significantly over the past two decades – and the government believes there are people being referred on to waiting lists who do not need treatment.
Streeting has previously suggested mental health conditions are being “overdiagnosed”.
Announcing the new review, Streeting said: “We must look at this through a strictly clinical lens to get an evidence-based understanding… That’s the only way we can ensure everyone gets timely access to accurate diagnosis and effective support.”
It comes as ministers seek to tackle a growing welfare bill – although the Department of Health and Social Care has stressed this review is running separately to that.
While some benefits require people to demonstrate how a health condition is affecting their ability to work, a formal diagnosis is not strictly necessary for many.
Earlier this year, the government was forced to climb down on planned cuts to disability benefits, including for those with mental health conditions, after facing major backlash from more than 100 of Labour’s own backbenchers.
But on Monday, the prime minister promised a renewed push on reforming the welfare system, which is said had “trapped people in poverty” and “wrote young people off as too ill to work”.
Led by clinical psychologist Prof Peter Fonagy, the new review’s findings will be published in Summer 2026.
Prof Fonagy said the aim was “to test assumptions rigorously and listen closely to those most affected, so that our recommendations are both honest and genuinely useful”.
NHS figures show that the number of adults aged 16 to 64 reporting mental health problems reached 22.6% in 2023-24, up from 17.6% in 2007.
Rates are higher in the young and among the unemployed.
As of March this year, around four million working-age adults in England and Wales claimed either disability or incapacity benefit – up from almost three million in 2019, according to research, external from the Institute for Fiscal Studies (IFS).
The DHSC said the increased pressure on the NHS “means that for too long, people with acute needs have faced long waits, had to navigate overstretched services, experienced inequalities in care and felt abandoned when support was needed most”.
The review will look at how NHS services are working and what support people could be given earlier.
Government sources said they wanted to establish a baseline for diagnosis and what good quality care looked like.
It is thought one of the factors in long waits was that people who did not necessarily need treatment were ending up being referred on to waiting list when practical support, such as help with social or financial issues or a short-burst of talking therapy could provide the solution.
Investment is already being made in increasing support in schools and expanding talking therapy services.
Royal College of Psychiatrists president Dr Lade Smith said: “We expect the review will adequately consider the many complex reasons that more people are in need of mental ill-health, ADHD and autism support.
“We have a real opportunity to ensure that millions of people receive the care they need both now and for generations to come.”
Mental health charity Mind welcomed the government’s announcement and signalled their willingness to contribute to the review.
“This is a huge opportunity to really understand what is driving increasing levels of mental illness, especially among our young people,” chief executive Dr Sarah Hughes said.
The National Autistic Society said: “We need urgent action because, while we are currently seeing the number of people seeking an assessment levelling out, the average waiting time is rocketing.”
Jack and the Beanstalk open air concert at the carnival
Sheriff With MND Uses Voice App To Speak In Court
A Dundee sheriff robbed of his voice by motor neurone disease (MND) is continuing to dispense justice from the bench with the aid of new technology.
Alastair Carmichael was diagnosed with the disease in early 2024, and now communicates with staff, lawyers and the accused using synthetic voice apps.
He is believed to be the only judge in the world currently conducting criminal jury trials in this manner.
The sheriff was speaking ahead of former rugby league star Kevin Sinfield arriving in Dundee on Saturday as part of his 7 in 7: Together ultramarathon challenge to raise money for MND research and treatment.
MND is a neurodegenerative condition where messages from the brain and spinal cord stop reaching the muscles.
High-profile cases include former Scotland international rugby player Doddie Weir, who died at the age of 52 in 2022, six years after being diagnosed.
The 62-year-old sheriff, who has sat on the bench in Dundee for a decade, said he first noticed “something was up” when he developed a persistent lisp in May 2023.
“The lisp didn’t go away as I had hoped it might,” he told BBC Breakfast.
“And then I found I was having to work a bit harder to get some consonants and words out.
“My oldest friend had MND and his voice had been affected so I suspected that something wasn’t right.”
The sheriff was initially reassured by his doctor that he did not have the condition, which affects about 480 people at any one time in Scotland.
He said: “However, she only had one symptom to go on, so I don’t blame her for not finding anything and at least it put my mind at rest for a few more months.”
After his symptoms progressed, he was referred to the neurology department at Ninewells Hospital, and ultimately diagnosed.
Unable to use his natural voice anymore at work, he has used an app called SpeakUnique to communicate in court for more than a year as he adjusts to what he calls “the new me.”
He said: “I have four different IT systems and I use them by having stored phrases that I can amend as needed and by also text to speak where I type in the letters and my synthetic voice says the words.”
“I think we’ve now come to the happy place where it’s just part of the furniture, and we can all just focus on the cases that are calling and on achieving justice in them.”
Sheriff Carmichael also uses visual cues in court, often pointing to the person he is about to address via the software to alert them.
He downplays the unique working situation he finds himself in.
“I have never claimed to be the only judge using text to speak IT in order to conduct criminal jury trials, but I am the only one we are aware of so far,” he said.
“With all the IT that is around it wouldn’t surprise me if there were other somewhere, it’s a big world.
“For example, employment judge Hugh Lumby who also has MND is using similar IT in his work in the London South region.
“It doesn’t really matter if I am the first or how many judges there are using this kind of IT.”
What does matter, he believes, is that it shows that people with the condition or other illnesses can continue to work, if adjustments are made to suit their situation.
He said: “This allows employers to retain experienced staff and consistency and allows people to continue to work and contribute to society. What’s not to like about that?”
The sheriff is determined to continue working for as long as he can.
He said: “Working gives me a focus away from MND and it allows me to feel like I am still participating in society.
“I always felt grateful for the start that I had in life, and have wanted to give something back by contributing to society.
“My job is a very public one, and continuing to work gives me the chance to show that even if you have lost your voice, you can continue to work with the assistance of voice IT and with the assistance of positive-minded people.”
‘Massive efforts’
He is full of praise for Kevin Sinfield’s charity challenge, saying the ex-rugby league star is doing “amazing things” for MND research and treatment.
Sinfield was inspired by, and continues to run in memory of, his former Leeds team mate, Rob Burrow, who was diagnosed in 2019 and died, aged 41, in June last year.
The sheriff said: “His massive efforts are helping to put him MND in the public eye and are helping to encourage people and organisations to give generously.
“This money is funding research and funding assistance, every penny helps to make things better now and in the future.
“He is also showing that if you set your mind to achieve something, then you can indeed achieve it. “
The sheriff said that his speech has now been affected to the extent that his family do not understand what he is saying, and his swallowing is now “less efficient.”
He said: “Beyond that, I am still mobile and can still do most things that I want to, although not necessarily in the same way as I used to.
“I must stress I could not have done this by myself.
“I’ve had help and support from my family, the medics, from the judges, from the court staff, and from the lawyers in court.”
He said that MND is a “nasty disease” that no one should have to face alone.
He said: “I am now far more reliant on other people than I used to be, and this is a humbling situation to be in.
“I’m lucky because the people who I work with have embraced risk and are willing to give it a go and see what happens.”
Singer Example Criticized For Telling Disabled Fans To Stand
British singer Example faced backlash after repeatedly demanding audiences stand and dance during performances on tour with boyband JLS, including telling a pregnant disabled fan she looked stupid for remaining seated. The incident at London’s O2 Arena sparked widespread criticism on social media and raised questions about accessibility awareness at live music events.
Elliot John Gleave, 43, who performs under the stage name Example, serves as the opening act for JLS on The Club Is Alive: 2025 Hits Tour. A video posted to TikTok showing the singer complaining about seated audience members has been viewed more than 45,000 times, according to the concertgoer who shared it.
The pregnant and disabled fan, posting as kxrstyyx on TikTok, wrote that getting called out by Example was not on her bingo card for 2025. The video captured the singer asking what audience members were doing and saying they looked stupid for not standing. The fan explained she was 27 weeks pregnant and disabled, making it necessary for her to remain seated during the performance.
Multiple concertgoers reported similar incidents at different venues throughout the tour. One attendee said that in Nottingham, Example complained the whole time about people being seated. Another wrote that he displayed similar behavior in Cardiff, appearing angry that everyone was sitting down.
The disabled fan revealed in comments on her TikTok post that at one point during the show, she held up her walking aid to indicate why she needed to sit. However, Example reportedly proceeded to call her stupid despite seeing the mobility device. This detail emerged when another follower commented that they remembered the camera showing her holding up the walking aid.
Supporters flooded the comments section expressing sympathy and sharing their own concerns. One person who identified as having chronic pain said they felt terrible for the concertgoer when the incident happened and expressed relief about not having front row seats. A wheelchair user commented that their boyfriend joked about Example telling them to get up and dance.
Another attendee at the O2 show stated they kept telling their group they didn’t like Example because he was being really rude during his performance. The consistent reports from multiple venues suggest the singer’s behavior represented a pattern rather than an isolated incident.
Example achieved commercial success between 2010 and 2013 with hits including Won’t Go Quietly, Kickstarts and Changed the Way You Kiss Me. The singer also had a number one single with Stay Awake and featured on Calvin Harris’s track We’ll Be Coming Back. His recent appearance on The Masked Singer as Bear helped remind audiences of his musical catalog and won him new fans.
The fan later told The Sun that after the concert, she met JLS members who treated her kindly. She said the boyband members were absolutely lovely, mentioning how they loved that she had painted her walking aid in matching colors. The contrast between Example’s behavior and JLS’s response highlighted different approaches to fan interaction and inclusivity.
JLS consists of Aston Merrygold, Oritsé Williams, Marvin Humes and JB Gill. The group became one of Britain’s biggest pop acts after finishing second on The X Factor in 2008 behind Alexandra Burke. They have sold over 10 million albums, scored five number one singles and won two BRIT Awards along with five MOBO Awards.
The group initially split in 2013 but reunited in 2020, launching their Beat Again Tour in 2021 after pandemic delays. Their subsequent tours in 2021 and 2023 filled arenas across the United Kingdom. The Club Is Alive: 2025 Hits Tour features their classic hits including Beat Again, Everybody In Love, The Club Is Alive, Love You and She Makes Me Wanna.
Example was personally invited by JLS to serve as special guest support for each show on the tour. In promotional materials, Example expressed excitement about performing on huge arena stages, describing performing as his bread and butter. He acknowledged that all the performers are getting older but promised the energy from everyone would be worth the ticket price.
The controversy highlights ongoing challenges regarding accessibility and awareness at live events. Many venues offer accessible seating and accommodations for disabled patrons, yet performers sometimes fail to recognize that not everyone can participate in standing or dancing. Medical conditions, disabilities, pregnancy and other factors legitimately prevent some audience members from standing for extended periods.
Concert etiquette has evolved as awareness of disabilities has increased, with many artists making efforts to be inclusive of fans with various accessibility needs. Some performers specifically acknowledge seated sections and encourage audience participation without requiring physical standing. Others create designated accessible areas where fans can enjoy shows without pressure to stand.
Social media has amplified accountability for performers whose comments or actions exclude disabled fans. Previous incidents involving artists demanding audiences stand have sparked similar backlash, with disability advocates emphasizing that invisible disabilities mean performers cannot determine who is capable of standing simply by looking at them.
The incident raises questions about whether Example will adjust his performance approach for remaining tour dates. Artists have previously apologized and changed their behavior after receiving feedback about accessibility issues. However, Example has not publicly commented on the criticism or the specific incident involving the pregnant disabled fan.
The tour continues through early 2025 with dates scheduled across multiple cities. JLS has built a reputation for engaging with fans and creating an inclusive atmosphere at their shows. Their positive interaction with the disabled fan after Example’s comments suggests the headlining act maintains different standards for fan treatment.
Disability rights advocates emphasize that accessibility extends beyond physical accommodations like ramps and designated seating. True inclusion requires awareness from all performers and staff that audience members have diverse needs and capabilities. Comments that shame or pressure people to stand can create hostile environments for disabled patrons who already face barriers to attending live events.
The video evidence and multiple witness accounts from different venues establish a pattern suggesting Example’s comments were not accidental or taken out of context. The repetition across multiple cities indicates the singer made similar demands of audiences throughout the tour rather than this being a single misunderstanding.
Music industry professionals note that opening acts face challenges energizing crowds who primarily came to see the headliner. However, most artists recognize that demanding physical responses from audiences proves counterproductive and potentially excludes fans with legitimate reasons for remaining seated. Building energy typically requires reading the room and meeting audiences where they are rather than imposing requirements.
The controversy may affect Example’s reputation and future booking opportunities as both venues and artists increasingly prioritize accessibility and inclusive fan experiences. Social media documentation of the incidents ensures the behavior remains part of public record, potentially influencing how promoters and fellow artists view collaborating with the singer.
For the pregnant disabled fan who shared the video, the experience of being called out and called stupid by a performer she paid to see left a negative impression that overshadowed the positive aspects of meeting JLS afterward. Her decision to share the video on TikTok brought attention to accessibility issues at concerts and generated conversations about how performers should treat all audience members with respect regardless of their ability to stand.